
Explore journal overview, editorial leadership, indexing, articles in press, latest published work, and highlights from previous issues.
Research Article :
A gradual decrease of the mortality
rate of infants and under five in the Philippines was recorded from 1996 to
2013. However, this sign of progress still requires additional efforts to
achieve the Millennium Development Goal of reducing the risk. This paper
attempts to test empirically the different factors affecting mortality rate of
infants and under five in the Philippines, an indicator in gauging health
security using a time series data (1996-2013). This will serve as a basis in
crafting policies that will critically and efficiently reduce the number of
deaths. The average mortality rate of infants and under five was selected as the endogenous
variable, Gross Domestic Product per capita and out of the pocket health
expenditure were treated as the exogenous variable. Health expenditure total
percentage of Gross Domestic Product and average percentage of immunization
were the mediating variables. Using structural equation modeling, all these
variables were tested for possible complex causality. Result showed that both
Average Immunization and Gross Domestic Product per capita significantly affect
mortality rate (β=-.510, p<.000; β=-1.340, p<.05). Thus, it is strongly
recommended that the country should critically undertake measures to increase
Gross Domestic Product per capita and should widen immunization rate. Mortality rate of
infants and under five serve as a more sensitive indicator of health security
across and within economies. Aside from being a factor associated with
population wellbeing, it also reflects improper childcare [1], state of public
health and hygiene, environmental sanitation, cultural mores about feeding and
clothing, socio-economic development, and above all, the peoples attitude
towards the dignity and value of human life itself [2]. Clearly public health conditions
and socio-economic wellbeing are greatly determined by infant and under five
mortality rate [3]. Globally, according to the United
Nations International Childrens Emergency Fund, it is estimated that there were
around 7 million under five deaths recorded with Sub-Saharan Africa as a major
contributor. Further 257 deaths per 1000 live births in Afghanistans for
under-five was recorded, third highest in the world, surpassed only by the
rates for Angola and Sierra Leone [4]. Even in other highly developed
countries, protecting human life is still a problem. The United States rate of infant mortality did
not decline from 2000 to 2005, 6.86 infant deaths per 1,000 live births, not
significantly different than the rate of 6.89 in 2000 higher than those in most
other developed countries [5] even in Canada with 5.1 in 2007 [6]. The Philippines is not spared of the
problems that countries abroad are facing. It was recorded that there were 64 deaths
per 1,000 live births in 1993 to 40 deaths in 2003 for under five children. A
study conducted by the National Statistics Office; a greater risk of dying is
associated to a child
born in the country as compared to other Southeastern Asian Countries
(NDHS, 2003) with 29 for every 1000 infants births die and
40 before reaching the age of five. In the case of under-five, the country will
be able to achieve the Millennium Development Goals (MDG) of reducing the
national U-5MR by two-thirds or only 19 deaths per 1,000 live births if the
trend will continue [7]. The research findings can be useful
value for the National Government to look into the possible major contributors
of mortality rate
of infants and under five in the country. Strengthening the sectors that
contributes significantly may also be given sufficient focus. Theoretical Background Economic theory The basic economic theory supports the study. This explains
that an increase in per capita income will lead to increases in the demand for
health care if everything else is held constant and if health care is a
normal good [8]. In this study, it is believed that when GDP per capita
increases, the budget allotted to health expenditure also increases so as
average percentage for immunization. Factors affecting mortality rate several studies were conducted to determine different
factors affecting mortality rate of infants and under five. And it is also
generally understood that some may influence positively or negatively. This
study emphasizes significant factors that may associate mortality rate. First,
it is hypothesized that GDP per capita is associated with health expenditure
total percentage of GDP per capita. That is, the proportion allotted for health
expenditure is affected by GDP per capita fluctuation. The country recorded the
highest GDP per capita (1995-2013) in 2013 with 2787 and with 958 as the lowest
in the year 2001. Several studies have confirmed that GDP per capita has a strong
negative effect to infant mortality rate [9,10]. Further, the health
expenditure total percentage of GDP per capita in the country is relatively
high with 4.42 percent of the GDP per capita in 2012 and lowest in 2002 which
accounted for only 2.80 percent. Musgrove [11] confirmed in his study that
private expenditure on health reduces child mortality. In this study, it is
hypothesized that GDP per capita and health expenditure total percentage of GDP
per capita affect mortality rate of infants and under five and that GDP per
capita affect health expenditure total percentage of GDP per capita. Second, it is hypothesized that out
of the pocket health expenditure affect mortality rate of infants and under
five. It is also essential to note whether out-of-pocket health expenditure (%
of private expenditure on health) affect mortality rate. The country received
the highest OOPHE in 2006 which accounted for 85.3 percent of the private
expenditure on health. Akinci et al. [12] revealed in their study that private
spending on health
significantly reduce infant and under five
mortality rates. Third, average percentage of
immunization of DPT and measles is associated to mortality rate of infants and
under five. Immunization is regarded to influence significantly the dependent
variable. Nyrako et al. [13] found out that Immunization can substantially
enhance child survival in high-mortality settings,
reducing mortality by up to two-thirds in children who receive the full package
relative to children
who have received no vaccinations. In 2013, the country recorded a highest
immunization percentage of 90.5 and lowest in 1995 with only 71 percent of
12-21 months children received DPT and measles vaccine. It is assumed that the
higher the percentage of immunization, the lower the rate of infant and under
five mortality rates. In this study, GDP per capita, HETPGDP and OOPHE are
assumed to influence average percentage of immunization. The following research questions
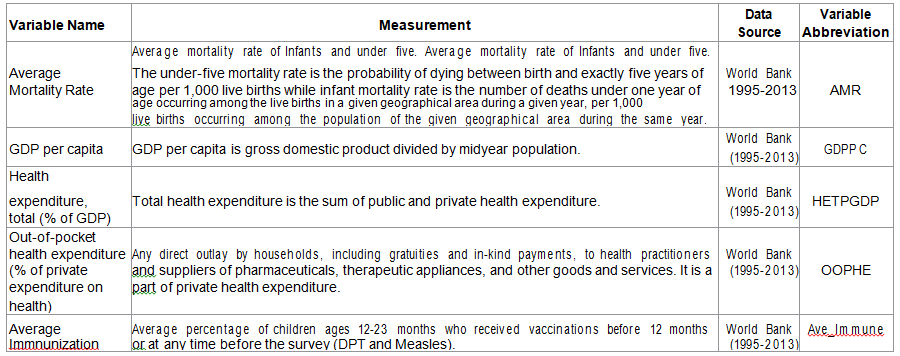
were formulated on the basis of the theoretical discussion above: Five independent variables and one
dependent variable were analyzed in the study. The independent variables
include: per capita DGP, Health expenditure (total percentage of GDP),
out-of-pocket health expenditure (% of private expenditure on health) and
average percentage of immunization of DPT and measles. Mortality rate was the
dependent variable. Please refer in the table below for the names of the
variables, the measurement and the data source (Table 1). First, descriptive statistics and
correlation coefficients for GDPPC, HETPGDP, OOPHE, Ave immune and AMR were
generated using SPSS version 20. Second, Analysis of Moment Structures (AMOS) 20.0 program was
carried out for structural equation modeling (SEM). In SEM, estimating
coefficients was channeled through Maximum Likelihood Estimation method.
According to Ingram et al, Maximum Likelihood Estimation (MLE) is an iterative
procedure that attempts to maximize the likelihood that obtained values of the
criterion variable will be correctly predicted unlike OLS that minimizes the
squared deviations between values of the criterion variable and those predicted
by the model. Since χ2is sensitive to sample size [14], and framing the null
hypotheses is often too difficult, both the χ2 and
fitness tests were used to evaluate model fitness. Goodness-of-Fit Index (GFI),
Comparative Fit Index and Normed Fit Index were also presented to evaluate
goodness of fit of the model. Third, modification index was also carried out to
find the optimal model for explaining the relationships among variables, in
case the hypothetical model projected will be proved not suitable. Fourth, the
mediating effects of HETPGDP and average percentage of immunization were tested
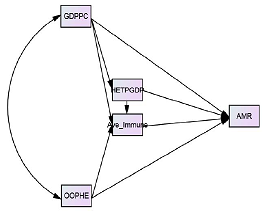
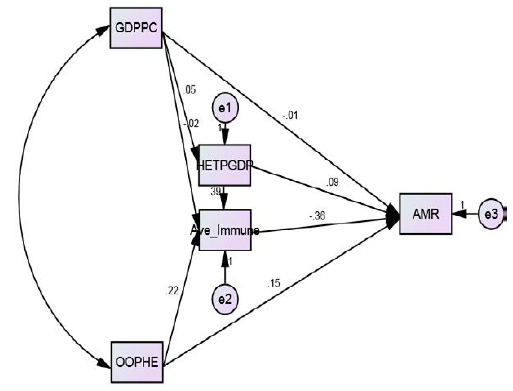
employing the bootstrap method. Presented below is the hypothetical
constructed model to test the possible exogenous variables that may possibly
affect mortality rate based on the theoretical points discussed. In this study, GDPPC and OOPHE were
treated as the exogenous variables and the rest of the variables were
endogenous (Figure 1). Presented in Table 2 is the
descriptive statistics of the variables used in the study. This includes the
minimum, maximum, means and the standard deviations. The data is reflective of
the countrys GDPPC, HETPGDP, Ave Immune, OOPHE and AMR. On the average, the Gross Domestic Product
Per Capita (GDPPC) for year 1995-2013 is 1512.56, 57.31 for health expenditure
total percentage of gross domestic (HETPGDP), 81.6 in the out of the pocket
health expenditure and an average immunization rate of 83.39 and 32.44 in the
average mortality ate. The data for average mortality rate is suggestive to
heighten significant measures that may
directly or indirectly influence on it (Table 2). Table 2: Descriptive Statistics. Presented in Table 3 is the
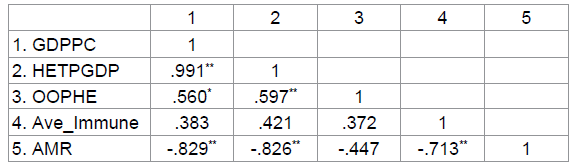
variables correlation included in the hypothetical model. The structure
hypothetically presents that the four endogenous variables are directly or
indirectly interconnected. In the final model, the following were found to be
significantly correlated: HETPGDP and GDPPC (r=.991, p<.01); OOPHE and GDPPC
(r=.560, p<.05); OOPHE and HETPGDP (r=.597, p<.01). For the dependent
variable, AMR and GDPPC (r=-.829, p<.01); AMR and HETPGDP (r=-.826,
p<.01); MR and Ave Immune (r=-.713, p<.01) were also found significant.
This means that the gross domestic product per capita is translated is
significantly translated into health expenditure
total percentage of gross domestic product which can also be significantly
translated from an increase in the Out- of the pocket health expenditure. An
increase in the percentage of immunization will significantly decrease the
average mortality rate of children (Table 3). Table 3: Variable Correlation. According to Gao et al, as cited in
Young-Chool Choi, Ji-Hye L [14] structural equation modelling does not have a
widely accepted measure of goodness of fit, thus this study follows the tests
explained by Ho [15] that includes chi square, GFI, CFI and NFI. Presented
below is the table for the goodness of fit of the hypothesized model (Table 4). Table 4: Goodness of Fit of the Model. As presented in Table 5, the model
fits the data well evident in the following measures of goodness of fit: χ2 =2.748
(p=.097); CFI=.985; GFI=.946 and NFI=.978. All values exceed the recommended
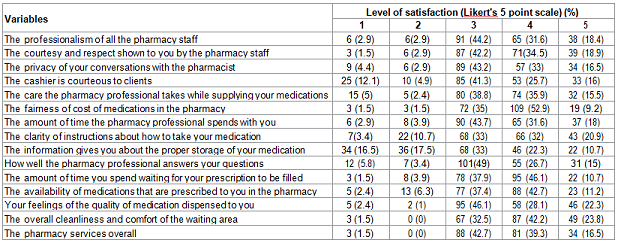
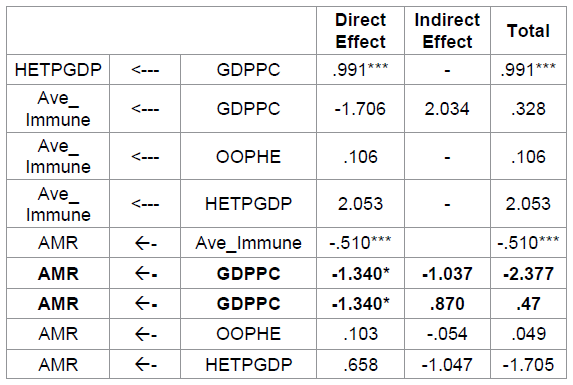
threshold and can be described as acceptable (Table 5), (Figure 2). Table 5: Independent Variables Affecting Mortality Rate. Figure 2: Structural Equation Model. As shown in Table 5, it was found
out that GDPPC significantly affects HETPGDP (β=.991; p=.000). More importantly
it resulted that GDPPC (β=.-1.340; p<.05) and ave immune (β=-.510;
p<.001) both affect mortality rate negatively. The direct effects of both
GDPPC and ave immune are the identified key structural paths. Their negative
sign implies that a higher rate of average percentage of immunization and
increase in GDP per
capita will reduce mortality rate. Both economic and health implications
can be extracted in the result to determine ways and means to increase GDP and
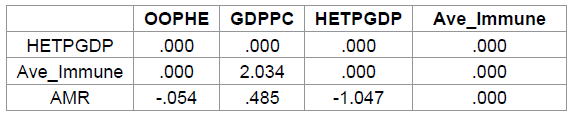
percentage of immunization. Table 6: Standardized Indirect Effects (Group number 1 - Default model). Table 6 shows the standardized
indirect effect or the as the index of mediation [16]. GDPPCs indirect effect
on Ave Immune is 2.034 and not significant p=.212, 95% CI [-2.831, 7.297], OOPHE
to AMR is still not significant (-.054), p=.866, 95% CI [-.327, .802]; HETPGDP
to AMR not significant (-1.047), p=.116, 95% CI [.000, .885], and GDPPC to Ave
Immune to Mortality
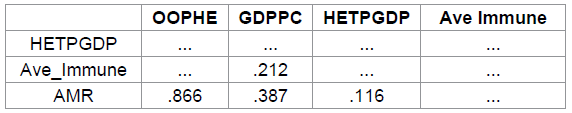
rate (.485), p=.387, 95% CI [-1.310, 3.434] is also not significant. Meaning, HETPGDP and Ave immune do
not significantly mediate the effect of GDPPC and OOPHE to AMR (Table 7). Table 7: Standardized Indirect Effects - Two Tailed Significance The central purpose of this endeavor
is to determine the causal complex connections between GDPPC, HETPGDP, ave
immune and OOPHE to the average mortality rate of infants and under five and to
craft policies that can help reduce incidence of mortality rate by employing
structural equation modeling technique. The study follows the requirements
using the statistical tool in specifying the model and in evaluating the
goodness of fit criteria. Estimating for the direct, indirect effect and total
effects was also carried out. Model fit indices include χ2 =2.748,
p=.097; GFI=.946; CFI=.985 and NFI=.978. Based on the set criteria study shows
that the generated model is statistically significant and can be described as
acceptable. The following implications are drawn out from the findings. First,
considering that the model including GDPPC negatively affect mortality rate,
there is a need to look into the significant determinants of increasing the
GDPPC. Second, since average percentage of immunization
significantly affect mortality rate, widening immunization for both DPT and
measles vaccination
should also be considered. This study will not claim that it
does not encounter the problem of empirical estimation. covers data from 1995-2013 which may
be considered as limited. A recommendation to cover years from 1980-2016 can be
considered. Second, it should also be noted that the study only focused in the
Philippines. Although the hypothetically projected model was proved
significant, the result may not be applicable to other countries. Third, the
study includes only limited number of variables, many variables may also affect
mortality rate but were not included in the conceptual
model. Maternal health
care, environmental conditions, access to improved sanitation and
nutritional status of the parents may also be considered. The whole idea of estimation is to
quantify the effects of GDPPC, HETPGDP, Ave Immune, and OOPHE to AMR. More
interesting results and valid conclusions could be drawn from a more a global study and for this
time may consider variables other economic and financial sectors. 1.
1. Zakir M, Wunnava PV. Factors
Affecting Infant Mortality Rates: Evidence From Cross-Sectional Data (1999)
Applied Economics Letters Pp: 271–273. Sherwin S. Fortugaliza, Davao City National High
School, Davao City, Philippines, Tel: (082) 227-9102 E-mail: sherwin.fortugaliza@yahoo.com Fortugaliza SS(2017) Factorsaffecting Mortality Rate of Infants and under Five in the
Philippines: An application of Structural Equation Modeling. NHC 119: 21-25 Infant and under five, Mortality
rate, structural equation modelingFactors affecting Mortality Rate of Infants and under Five in the Philippines: An application of Structural Equation Modeling
Sherwin S Fortugaliza
Abstract
Full-Text
Introduction
Research Questions
Research Designs Variables
Analysis method
Hypothetical model
Results
Descriptive statistics

Correlation of the variables
Goodness of Fit
SE Model
Conclusions and Policy Implications
Limitations of the Study
References
2.
Bawa AA. Living standards, household
size and childhood survival in Africa: Evidence from Census Data (2001)
University of Pennsylvania, Population Studies Center, Philadelphia.
3.
Miller NZ, Goldman GS. Infant
mortality rates regressed against number of vaccine doses routinely given: Is
there a biochemical or synergistic toxicity? (2011) Hum Exp Toxicol 30:
1420–1428.
4.
Adedini. Regional Variations in
infant and child mortality in Nigeria: A Multilevel Analysis (2015) Journal of
Biosocial Science 47: 165-187.
5.
MacDorman. Recent Trends in Infant
Mortality in the United States (2008) NCHS data brief, National Center for
Health Statistics Hyattsville, MD, USA.
6.
Infant Mortality (2016) Conference
Board of Canada.
7. Infant Mortality in the Philippines is Higher than Other Southeast Asian
Countries (2004) Philippine Statistics Authority.
7.
Day K, Tousignant J. Health
Spending, Health Outcomes and Per Capita Income in Canada: A Dynamic Analysis.
(2005).
8.
Upadhyay KA, Srivastava S.
Association between Economic Growth and Infant Mortality: Evidence from 132
Demographic and Health Surveys from 36 Developing Countries (2012)
International
Institute for Population Sciences
Mumbai, India.
9.
Wheatley, Lisa. Factors affecting
child mortality (2015) Honors Theses.
10.
Musgrove P. Public and Private Roles
in Health: Theory and Financing Patterns (1996) Health, Nutrition and
Population (HNP) Discussion Paper, World Bank.
11.
Akinci. Examining the Impact of
Health Care Expenditures on Health Outcomes in the Middle East and North Africa
(MENA) Region (2014) Journal of Health Care Finance.
12.
Nyarko. Immunization Status and
Child Survival in Rural Ghana (2001) Policy Research Division Working Paper
#147.
13.
Young-Chool Choi, Ji-Hye L.
Analyzing the relationships among the factors affecting educational
competitiveness: An application of the structural equation modeling approach
(2014)
Journal of Arts and Humanities 3:
40-50.
14.
Ho Robert. Handbook of Univariate
and Multivariate Data Analysis with IBM
(2014) CRC Press Taylor & Francis Group FL USA.
15.
Preacher KJ, Hayes AF. Contemporary
approaches to assessing mediation in communication research (2008a) In: The
Sage sourcebook of advanced data analysis methods for
communication
research AF Hayes, MD Slater, LB
Snyder (Edtrs.) Thousand Oaks, CA, Sage, Pp: 13–54.*Corresponding author
Citation
Keywords