Introduction
Fear and anxiety whilst visiting a dentist for dental treatment is one of the most significant problems for majority of children and adolescents [1]. This fear in pediatric patients results in avoiding dental treatment and which negatively influences the patients oral health even in the future [2]. Systematic desensitization is an integral component of behavior guidance in pediatric patients as it is a behavioral therapy that helps to minimize fear and anxiety of the patient by helping them to relax and moving from less to more invasive procedures [2].
Local anesthesia is used in dentistry to combat dental pain which facilitates the treatment for the patient and the dentist as well, however, the injection of a local anesthetic itself adds on to the fear of the patient as the sight of the needle is usually associated with pain and discomfort [3]. Hence it is the responsibility of the clinician that they do the best possible to minimize pain and discomfort during dental treatment [3]. Since needle phobia has become an obstacle for pediatric patients, various advancements to overcome this fear have been developed over the years inclusive of buffering Local Anesthesia (LA), precooling the site of injection, applying topical anesthesia, vibration or pressure at the site of injection and associated structures [4-6]. Devices like vibraject, accupal or jet injectors have been also used which are considered to be painless in nature when administering local anesthesia [7,8].
The present study was designed to compare three techniques which were applied before or during administration of LA. The procedure chosen in this study was dental extractions. As mentioned earlier, the tested techniques included the application of topical anesthesia before the administration of LA, precooling with ice before administration of LA and use of vibrations with powered toothbrush at the injection site during the administration of LA. The objective of this study was to determine the most effective method of painless anesthesia amongst the three selected techniques.
Materials and Methodology
The study was conducted at RAK College of Dental Sciences, Faculty of dentistry, RAK Medical and Health Sciences University, UAE. The study was conducted after obtaining the approval of the ethical board RAK Medical and Health Sciences Research and Ethics Committee respectively. A strict inclusion and exclusion criteria was followed for the research.
It was made sure that the children were medically fit, cooperative and the patients who had visited the clinics before as well, as the design of the present study wanted children who were less anxious as the procedure they were subjected to was dental extractions. Frankl behavior rating scale was used to determine the behavior of patients who belonged to the definitely positive category were included into the study. While selecting the procedure of extraction, it was made sure that the study would include patients who needed lower molar extractions and would be given inferior alveolar nerve block which would be uniformly followed for all patients in the study so as to keep the procedure uniform in nature so that there would be no other factors influencing the outcome of the research. Children who would require more than one cartridge of Local Anesthesia (LA) would be excluded from the study. Subjects who were included in the study were not on any medications, which could influence the results.
Initially all the children and parents who were willing to participate in the study were invited and pooled as a group. This allowed the parents and the children to decide if they wanted to participate in the study or not. 106 children and their parents were recruited in the study considering a possible attrition rate in due course. Once the children and parents were pooled then a presentation regarding the study was made to the selected population. Out of these 34 children and their parents withdrew from the study after the presentation, and 18 children retracted from the study as the children became uncooperative on the dental chair. Finally we had a sample size of 54 children who belonged to the age groups of 6-13years who fit the selection criteria and completed the study.
A simple randomization was done using a lottery system to divide the whole population into three groups. The chits were placed in a bowl with Group I, Group II and Group III written on them. The children were distributed according to these chits (Figure 1). The technique of pre anesthesia was as follows:
Group I-Topical Anesthesia was applied at the injection site for 1 minute and then local anesthesia was administered.
Group II-Precooling with ice at the site of anesthesia for 1 minute followed by Local Anesthesia (LA) administration.
Group III-Vibrations from a powered toothbrush at the injection site during administration of LA.
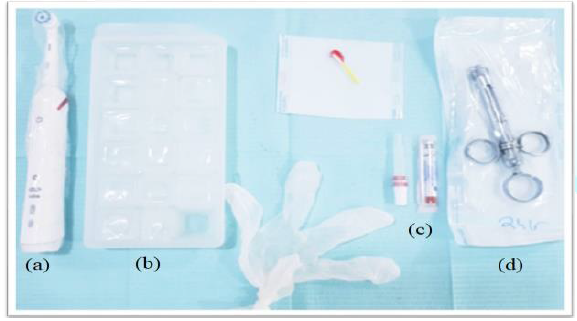
Figure 1:
Armamentarium used for the research.
Powered toothbrush (b) Ice cubes (c)
Topical anesthesia gel (d) Local Anesthesia Syringe.
Statistical Analysis
Wong Baker scores were tabulated and analyzed using SPSS version 20. Statistical analysis was done using Chi square test. Mann Whitney test was done for comparison between groups. Chi square test was used to compare the distribution of scores between the three groups. Mann Whitney was used for pair wise comparison of the Wong Baker Faces Pain Rating Scale score between the groups. The results were considered statistically significant if the p value is ˂0.05.
Results
The three groups involved in the study were divided based upon the technique of pre-anesthesia used to reduce pain during LA administration. In the present study it was found that the best pain reduction was seen in vibrations group with the Wong Baker Faces Pain Scale scores being at 1.33 and the least pain reduction was seen in the group where topical anesthesia was applied at 4.67 and the results were statistically significant (p˂0.003) (Table 1 and Figure 2).
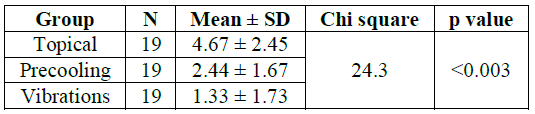
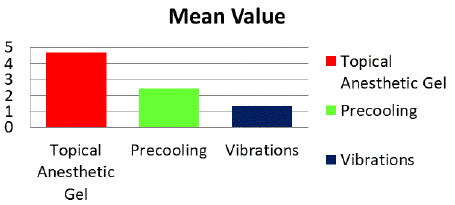
Figure 2: Comparison of mean pain scores of the three groups of pre anesthesia.
When a comparison was made among the groups, it was found that all the comparisons were statistically significant. However, the vibrations group was found to have a higher significant result statistically (p˂0.0001) (Table 2).

Table 2: Mean pain scores when compared between groups when paired.
Discussion
It is understood that fear and anxiety are two important components which keep children away from dentistry and various techniques have been used to overcome this over a period of time. Behavior guidance or modification has been useful to a certain extent. Since local anesthesia administration is one of the most fear and anxiety provoking procedures, clinically innovative methods of administering LA have also been considered in some researches. In the present study the authors have compared three types of possible pre-anesthesia methods like application of topical anesthesia before administering LA, precooling the site of injection before application of LA and the application of vibrations during the process of LA.
Topical anesthesia has always been a routine in pediatric dental clinical practice [8]. In the present study we found that the mean scores of Wong Baker Faces Pain Rating (WBFPR) scale for topical anesthesia gel was 4.67 (Table 1, Group1) and was found to be higher than the other two groups (Table 1). It may be presumed that the unpalatable taste or burning sensation after applying topical anesthesia could be responsible for these high scores. In a research conducted by Guilherme Camponogara de Freiras it was concluded that topical anesthetic and the placebo had similar effects on pain perception for injection of local anesthesia [9].
The second group within the present study was subjected to topical cold application which is also found to increase the pain threshold. The application of cold over any site is expected to stimulate myelinated A fibers which thereby activate the inhibitory pain pathways. The results of our study suggested that precooling with ice reduces the fear and anxiety as seen in the reduction of mean WBFPR scores at 2.44 (Table 1, Group 2). Similar results were seen in a study conducted by Naser Asl Aminabadi that shows that cooling of the injection site of a nerve block prior to administration of local anesthesia significantly reduced the pain perceived by pediatric patients [10].
The third group of the present study was subjected to vibrations adjacent to the site of injection of LA. The Gate Control Theory of pain suggests that pain can be reduced by simultaneous activation of nerve fibers that conduct non noxious stimuli. The present study investigated the effects of vibration stimuli on pain experienced during local anesthetic injections.The vibrations were induced with the help of a powered toothbrush. The toothbrush was pouched using disposable sleeves during the process. The results showed the mean score of WBFPR scores at 1.33 suggesting that vibrations reduced the pain felt by the patients (Table 1, Group 3). Similar findings were reported in other studies where they found vibrations to be effective in pain control when compared to other pre-anesthetizing methods [7].
Some of these studies used vibro-tactile device, VibraJect, and reported similar findings as in the present study. It was also found that vibrations were more effective in pain control when compared to other pre-injection anesthetizing methods, although lesser than that of topical cold application. However, the study by those authors involved extra-oral vibrations which may be the reason behind the difference between results observed in their study and the present study [3,7]. Practitioners around the world use different means to reduce the pain whilst administering local anesthesia. Certain studies have shown a positive correlation between injection pressure, rapidity of injection and pain. It was concluded that local anesthesia be injected under low pressure and at a less rapid rate to minimize pain among dental patients [11]. Hence it is understood that administering the local anesthesia at a slow pace can make the injection virtually painless [12]. There were also other methods reported to reduce the pain during the injection of local anesthesia. These included buffering local anesthesia with sodium bicarbonate and also warming the local anesthesia prior to injection [9,13].
Although various other scales are available to assess pain, including faces pain scales specially formulated for use with young children, the Wong Baker FPR Scale was chosen due to its repeatability, ease of use with the age group involved in the study and the fact that it has been used in many past researches with significant positive correlation, asserting its reliability to assess perceived pain [14].
It is widely accepted that there are different methods of reducing pain and anxiety in pediatric patients but methods like use of euphemisms, distractions, voice control have played an important role in allaying fear and anxiety. However, reducing pain while injecting anesthesia is of prime importance and this was the focus of present study. In this study it was found that the three methods used did definitely decrease the pain during injection but vibrations created using the powered toothbrush gave the most statistically significant and cost effective results.
Conclusions
From this study we concluded that application of vibrations at the injection site was most effective in reducing the pain perception in pediatric patients.
References
1. Gao X, Hamzah SH, Yiu CK, McGrath C and King NM. Dental fear and anxiety in children and adolescents: qualitative study using YouTube (2013) J Med Internet Res 15: e29. https://doi.org/10.2196/jmir.2290
2. Garret-Bernardin A, Cantile T, DAntò V, Galanakis A, Fauxpoint G, et al. Pain experience and behavior management in pediatric dentistry: a comparison between traditional local anesthesia and the wand computerized delivery system (2017) Pain Res Manag 7941238. https://doi.org/10.1155/2017/7941238
3. Aminah M, Nagar P, Singh P and Bharti M. Comparison of topical anesthetic gel, pre-cooling, vibration and buffered local anesthesia on the pain perception of pediatric patients during the administration of local anesthesia in routine dental procedures (2017) IJCMR 4: 77-83.
4. Davies RJ. Buffering the pain of local anaesthetics: a systematic review (2003) Emerg Med 15: 81-88.
https://doi.org/10.1046/j.1442-2026.2003.00413.x
5. Mohiuddin I, Setty JV, Srinivasan I and Desai JA. Topical application of local anaesthetic gel vs ice in pediatric patients for infiltration anaesthesia (2015) JEMDS 4: 12934-12940.
https://doi.org/10.14260/jemds/2015/1866
6. Hutchins HS Jr, Young FA, Lackland DT and Fishburn CP. The effectiveness of topical anesthesia and vibration in alleviating the pain of oral injections (1997) Anesth Prog 44: 87-89.
7. Blair J. Vibraject from ITL dental (2002) Dent Econ 92: 90.
8. Sriram G. Advances in local anaesthesia: A paediatric overview (2014) Indian J Dental Advancements 6: 1605-1607.
9. de Freiras GC, Pozzobon RT, Blaya DS and Moreira CH. Efficacy of benzocaine 20% topical anesthetic compared to placebo prior to administration of local anesthesia in the oral cavity: a randomized controlled trial (2015) Anesth Prog 62: 46-50.
https://doi.org/10.2344/0003-3006-62.2.46
10. Aminabadi NA and Zadeh Farahani RM. The effect of pre-cooling the injection site on pediatric pain perception during the administration of local anesthesia (2009) J Contemp Dent Pract 10: 43-50.
11. Kudo M. Initial injection pressure for dental local anesthesia: effects on pain and anxiety (2005) Anesth Prog 52: 95-101.
https://doi.org/10.2344/0003-3006(2005)52[95:IIPFDL]2.0.CO,2
12. Strazar AR, Leynes PG and Lalonde DH. Minimizing the pain of local anesthesia injection (2013) Plast Reconstr Surg 132: 675-684. https://doi.org/10.1097/PRS.0b013e31829ad1e2
13. Aravena PC, Barrientos C, Troncoso C, Coronado C and Sotelo-Hitschfeld P. Effect of warming anesthetic on pain perception during dental injection: a split-mouth randomized clinical trial (2018) Local Reg Anesth 11: 9-13.
https://doi.org/10.2147/LRA.S147288
14. Kumar M, Chawla R and Goyal M. Topical anesthesia (2015) J Anaesthesiol Clin Pharmacol 31: 450-456.
https://doi.org/10.4103/0970-9185.169049
*Corresponding author
Vivek Padmanabhan, Assistant Professor, Pediatric and Preventive Dentistry, RAK College of Dental Sciences, RAK Medical and Health Sciences University, United Arab Emirates, E-mail: vivek_pdr@rediffmail.com
Citation
Padmanabhan V, Hameed A and Sheikh AH. Comparison of three different techniques to allay anxiety before local anesthesia injection in pediatric population (2019) Dental Res Manag 3: 74-76.
Keywords
Topical anesthetic gel, Pre cooling, Toothbrush, Wong-Baker faces pain rating scale.


 PDF
PDF