Introduction
Curcumin is an herb with powerful anti-oxidative, anti-inflammatory, anti-mutagenic, and anti-microbial properties [1-9]. Oxidative stress can lead to chronic inflammation. Curcumin can decrease TNF-α production and can inhibit inflammatory cytokines. See for extensive reviews the studies of Pulido-Moran [10-20]. Because of these properties, curcumin has been studied in inflammatory diseases in lungs, joints, bowels, brains, and the cardiovascular system, rheumatoid arthritis, inflammatory bowel disease, Alzheimers disease, mood disorders, cancer, diabetes, pain. Although animal Experimental studies are overwhelmingly positive, there is only limited data from human studies [21-27].
Myalgic Encephalomyelitis/Chronic Fatigue Syndrome (ME/CFS), is a chronic and often disabling disease. The exact prevalence is unknown but estimates in the US vary between 836.000 and 2.5 million patients, in the Netherlands between 20.000 and 80.000 patients. Patients with ME/CFS have been found to be more functionally impaired than those with other disabling illnesses [28-30].
Although the exact pathophysiological mechanism of ME/CFS is unknown, immunological abnormalities may play an important role. Oxidative stress is increased in ME/CFS patients. The data on cytokines are contradictory and a recent meta-analysis showed no overall change for approximately 80 plasma cytokines studied in ME/CFS patients compared to controls. We previously showed in an open treatment trial that curcumin has favorable effects on symptomatology in ME/CFS patients, possibly because of the anti-oxidative and anti-inflammatory properties of curcumin. In the present study we hypothesized that effects in patient reported outcomes might be dependent on the severity of the disease [31-37].
Patients and Methods
Patients with ME/CFS were asked to participate in the registry and gave informed consent. All fulfilled the Fukuda criteria for CFS and the ME criteria. Disease severity was scored according to the ME criteria as mild, moderate, or severe. For this analysis, patients with moderate and severe disease severity were grouped together and compared with those who had mild disease [38,39].
Patients were asked to complete the CDC inventory for assessment of Chronic Fatigue Syndrome, Dutch language version, prior to the start of using curcumin and return the questionnaire by mail or email. After 8 weeks of curcumin use, the same questionnaire was completed. Prior to the start of curcumin they also completed the SF-36 questionnaire [40-42]. Patients used Curcumin Phytosome (Curcuma longa extract complexed with phosphatidylcholine; NOW®) 500 mg capsules twice a day. According to the manufacturer the capsules contained at least 18% (90 mg) curcuminoids.
In total 65 patients participated. Six patients stopped the use of curcumin because of side effects (all of gastro-intestinal origin). Eight patients did not return the second questionnaire despite two reminders. These 14 participants were excluded from the analysis, leaving 51 participants with complete data. No other treatments for ME/CFS were used during this study period. No side-effects were reported in the patients who completed the trial period and returned the second questionnaire. The work described has been carried out in accordance with The Code of Ethics of the World Medical Association (Declaration of Helsinki) for experiments involving humans. The medical ethics committee of the Slotervaart Hospital, Amsterdam, NL, approved the use of patient data for research (code U/17.089/P1736).
Data analysis
The CFS CDC inventory contains 19 symptom questions and collects information about the presence, frequency, and intensity of 19 illness-related symptoms during the month preceding the interview; these symptom questions include all the CFS-defining symptoms. Perceived frequency of each symptom was rated on a five-point scale (0-4) and severity or intensity of symptoms was measured on a four-point scale (0-3). Individual symptom scores were calculated by multiplying the frequency score by the intensity score. For this purpose the intensity scores were transformed into equidistant scores (0, 1, 2.5, and 4) before multiplication. This results in a range of 0–16 for each symptom [40].
The CDC score contained the summed score of the 19 symptoms. For the purposes of this analysis, we subdivided the CDC score into 2 parts: the CFS score and the CDC other score. The CFS score consisted of the 8 CFS defining symptoms namely, post-exertional fatigue, unrefreshing sleep, problems remembering or concentrating, muscle aches and pains, joint pains, sore throat, tender lymph nodes and swollen glands and headaches. In the CFS diagnostic criteria memory and concentration difficulties are taken as one combined symptom, whereas in the CDC inventory these 2 symptoms are scored separately. Therefore, for the CFS scores 9 symptoms were summed. The 10 remaining CDC questions that were not related to the CFS score were also summed and labeled as CDC-Other score. The CDC other score is composed of the symptoms: diarrhea, fever, chills, sleep problems, nausea, stomach or abdominal pain, sinus or nasal problems, shortness of breath, light hypersensitivity and depression.
Moreover, in the second, post-curcumin questionnaire, we asked how you rate your global physical and mental condition after using curcumin: 0: strongly deteriorated, 1: mildly deteriorated, 2: no change, 3: mildly improved and 4: strongly improved. One patient reported mild deterioration after curcumin use. For the chi-square analysis this Patient was added to the no change group. Similarly, the two improvement answers were also analyzed together.
Statistical Analysis
Scores were tested for normal distribution using the Shapiro-Wilk test in SPSS (IBM SPSS version 21). Normally distributed data are presented as mean (SD) and non-normally distributed data as median (IQR). Data were compared with Students test for paired and unpaired data, and with the Mann-Whitney U test for non-normally distributed data, where appropriate. Chi square analysis was performed on the distribution of the Patient Reported Outcome Measure (PROM): yes or no change in physical and mental condition after curcumin use. A p value <0.05 was considered significantly different.
Results
Table 1 shows the demographic data for the 51 participants analyzed. Forty-two females and 9 males were included. The mean disease duration was 16 (9) years, and the mean age was 47 (11) years. Except for height and weight, there were no differences between males and females (data not shown).
According to the ME criteria 26 patients were graded as mild and 25 as moderate to severe (15 moderate and 10 severe patients). Table 1 also shows the baseline data for the mild vs the combined moderate and severe group. No differences were present except for the SF-36 physical functioning scale; as expected, mildly affected patients had a higher physical functioning scale than the moderately and severely affected patients p<0.0001.
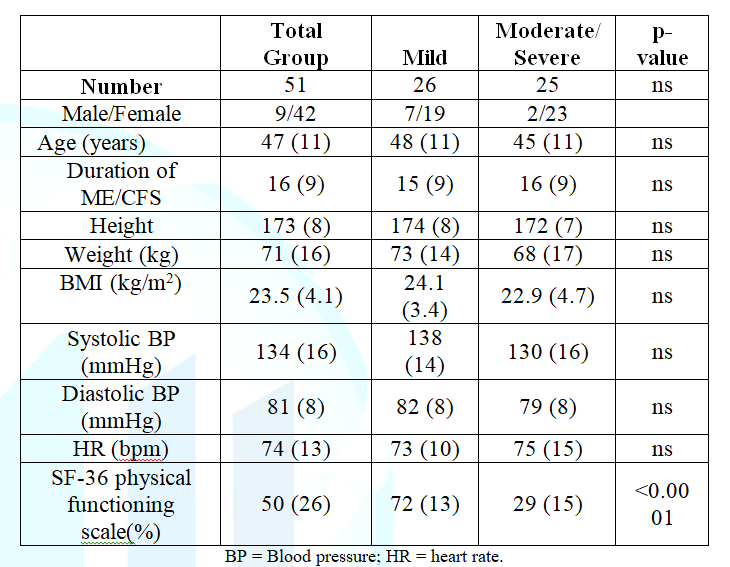
Table 1: Baseline characteristics of the total group and of the mild vs the moderate to severe ME/CFS patients.
Table 2 shows the CDC inventory score results and the PROM: the change in physical and mental condition after curcumin use.
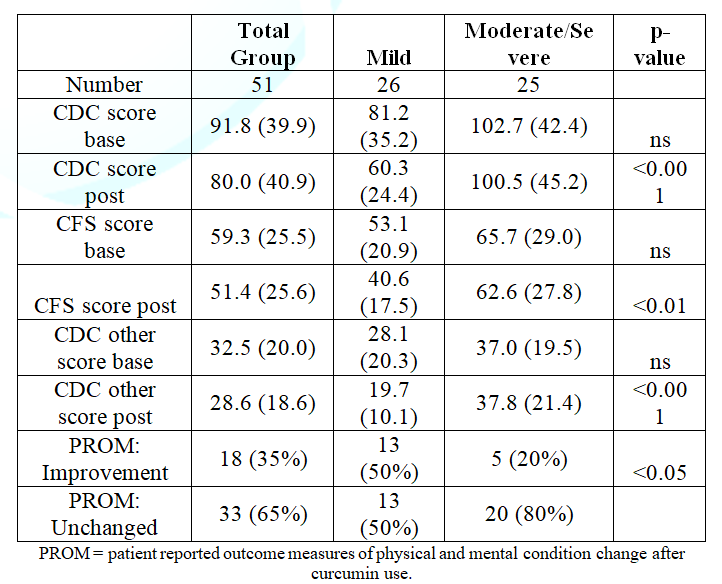
Table 2: CDC, CFS and CDC other scores for mild vs moderate/severe ME/CFS patients.
Figure 1 shows the data of the PROM: unchanged and improved physical and mental improvement versus the change in the total CDC score (post curcumin use minus pre curcumin use). Patients with the PROM: unchanged showed a significantly lower change in the total CDC score compared to the change in patients reporting improvement
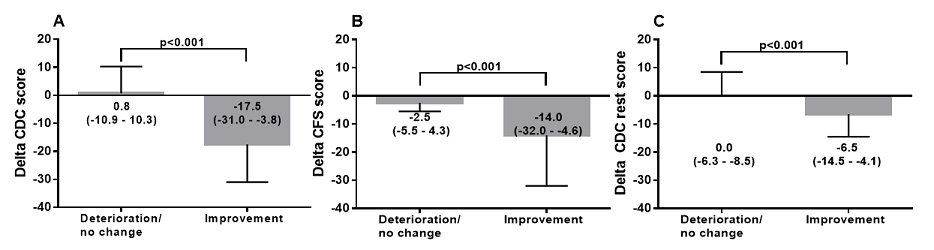
Table 2 also shows the differences between patients with mild disease vs moderate and severe disease. Baseline CDC, CFS and CDC other scores were all higher in the mildly affected patients versus the moderate and severe patients, but did not reach statistical significance. After 8 weeks of curcumin use, both the total CDC scores, the CFS scores and CDC-other scores were significantly lower (p<0.001, p<0.01 and p<0.001 respectively), compared to pre-curcumin use in the mild ME/CFS group, but were not different in the moderate to severe ME/CFS group.
Figure 1 show the changes in CDC, CFS and CDC other scores with respect to the patient reported outcome of neutral/deterioration or improvement. Figure 2 shows the pre- and post-treatment values of the three scores in both mild versus moderate to severe ME/CFS patients. The CDC, CFS, and CDC-other scores post curcumin use were all significantly lower in the mild ME/CFS group, whereas not different in the moderate to severe ME/CFS group.In the group with mild disease (n=26) 13 reported improvement in the global physical and mental condition, 13 reported no change. In the moderate/severe group, 5 reported improvement and 20 reported no change (p<0.05).
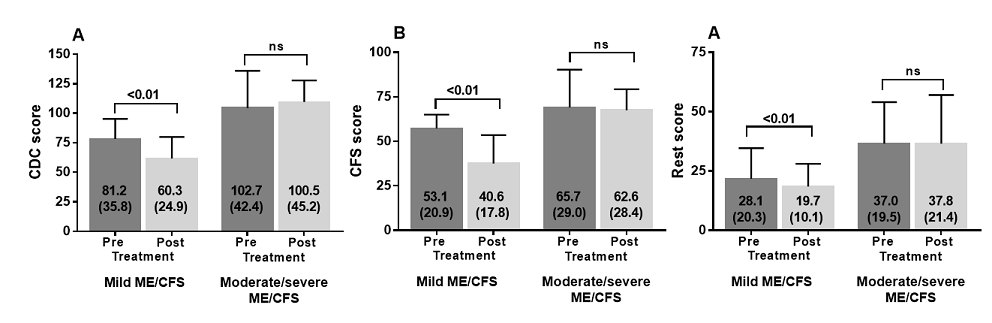
Figure 2: CDC score pre and post treatment in mild and moderate/severe ME/CFS patients (panel A), CFS score pre and post treatment in mild and moderate/severe ME/CFS patients (panel B) and CDC rest score pre and post treatment in mild and moderate/severe ME/CFS patients (panel C).
Discussion
To the best of our knowledge, this is the first study that indicates that curcumin use has a positive effect on symptoms in ME/CFS patients as assessed by the CDC inventory for CFS, and that those with more severe disease are less likely than those with mild disease to report improvement. In 2018 we published the first open label results in ME/CFS patients, showing curcumin might be a supplement to be prescribed in ME/CFS patients(van Campen 2018). In this larger group we investigated whether there was a relation between disease severity and efficacy.
Symptoms in ME/CFS include a perpetual flu-like state, sore throats, tender/swollen lymph nodes, muscle pain, achy joints without swelling or redness, headaches, chills, feverishness and sensitivities to foods, odors, and medications, which are all indicative of inflammation [28]. As increased oxidative stress and altered cytokine patterns have been demonstrated in ME/CFS, it is likely that curcumin exerts its beneficial effects by the anti-oxidative and anti-inflammatory properties. However, the exact mode of action of curcumin needs to be determined. Moreover, ME/CFS is considered to be in part a neuro-inflammatory disease. As curcumin passes the blood-brain barrier it is therefore tempting to assign the positive effects also to an anti-oxidative and anti-inflammatory effect in the brain [1-6,31-36,43-49].
Overall, the effect of curcumin use on ME/CFS symptoms is limited: for the total ME/CFS patient group the total CDC score decreased from 91.8 (39.9) to 80.0 (40.9), a mean reduction of 12% (data not shown). The limited efficacy is also obvious from the PROM: change in physical and mental condition after curcumin use. Thirty-five percent of patients reported improvement in their physical and mental condition after curcumin use. The finding that the PROM: improved is associated with a larger decrease in the total CDC score strengthens the validity of this study.
A difference in treatment efficacy was found between patients with mild disease versus moderate or severe disease. In the latter group curcumin was less effective. This observation is not uncommon in other diseases. For example, in a study using a bronchodilator for COPD (Chronic Obstructive Pulmonary Disease), the medication under study was less effective in severe COPD vs moderate COPD [50].The reduced efficacy in the moderate to severe ME/CFS patient may be related to a higher load of inflammation in this patient group in combination with the low bioavailability of curcumin. In the unprocessed form the uptake of curcumin is very low. To improve uptake, encapsulation in liposomes, polymeric nanoparticles, cyclodextrin encapsulation, lipid complexes, phosphatidylcholine complexes or polymer-curcumin complexes have been developed, all of which increase the activity and bioavailability. In a study the absorption of a standardized curcuminoid mixture and its lecithin formulation was compared [19,51,52].
Total curcuminoid absorption was about 29-fold higher than for its corresponding unformulated curcuminoid mixture, but plasma concentrations were still significantly lower than those required for the inhibition of most anti-inflammatory targets of curcumin. Remarkably, the phospholipid formulation increased the absorption of demethoxylated curcuminoid much more than that of curcumin, being a more potent analogue in many in vitro anti-inflammatory assays. It is possible that an even higher dose or an increased bioavailability of curcumin and or demethoxylated curcuminoid may be more effective in moderate to severe ME/CFS patients. These needs to be studied and further efforts to increase bioavailability and the clinical effects of the different curcuminoid components are also needed.
An interesting finding was that not only the CFS score decreased significantly in the mild disease group, but also the CFS-other scores. Some of these symptoms might be related to inflammation and therefore might respond to curcumin treatment. A larger study is needed to address the question regarding which specific symptoms are ameliorated by curcumin. Unexpectedly, a relatively high number of ME/CFS patients (n=6, 10%) stopped the use of curcumin because of side effects. The explanation may be that multiple chemical sensitivities are prevalent in ME/CFS patients. In the study of Brown and Jason, the co-occurrence was almost 24% [53]. It is unclear whether the drug itself or added excipients cause the intolerance. The patients completing the study reported no side effects due to this supplement.The meta-analysis of reported nausea and gastro-intestinal side effects to be the main reported adverse events. They also reported studies no showing any side effects. The ME/CFS patients with side effects found these severe enough to stop the treatment [54].
Limitations
This study was an open-label study, without a placebo arm. Some patients (n=8) did not return the first or second questionnaire, possibly leading to bias. A number of patients in the outpatient clinic admitted that they had difficulties with completing the questionnaire. This is most probably due to their memory and concentration problems, a disabling feature of the disease. A supervised completion approach may overcome this problem. The meta-analysis of table 1 shows an overview of trials in which there were different doses and durations of treatment, varying from single dose interventions up to treatment durations of 22 months [54]. We chose – empirically in the ME/CFS patient group – for treatment duration of 8 weeks. If a positive response is not present after 8 weeks, the likelihood that improvement will occur with longer duration is considered to be low. As patients are not reimbursed for these supplements, we elected to stop treatment after a few months. Further study would determine whether a longer duration might increase the percentage of responders.
Conclusion
In summary, in this open-labeled study, 8 weeks of curcumin use in a phosphatidylcholine complex reduced ME/CFS symptomatology, especially in patients with mild disease, whereas it did not significantly change symptoms in moderate and severe patients. A randomized placebo-controlled, larger study is warranted to assess its efficacy in ME/CFS patients.
Data Availability Statement
The raw data supporting the conclusions of this manuscript will be made available by the authors, without undue reservation, to any qualified researcher.
Acknowledgments
We acknowledge Prof PC Rowe for a critical review of the paper.
References
1. Joe B and Lokesh BR. Role of capsaicin, curcumin and dietary n-3 fatty acids in lowering the generation of reactive oxygen species in rat peritoneal macrophages (1994) Biochim Biophys Acta 1224: 255-263. https://doi.org/10.1016/0167-4889(94)90198-8
2. Reddy A C and B R Lokesh. Effect of dietary turmeric (Curcuma longa) on iron-induced lipid peroxidation in the rat liver (1994) Food Chem Toxicol 32: 279-283. https://doi.org/10.1016/0278-6915(94)90201-1
3. Kang J, Chen J, Shi Y, Jia J and Zhang Y. Curcumin-induced histone hypoacetylation: the role of reactive oxygen species (2005) Biochem Pharmacol 69: 1205-1213. https://doi.org/10.1016/j.bcp.2005.01.014
4. Jeong GS, Oh GS, Pae HO, Jeong SO, Kim YC et al. Comparative effects of curcuminoids on endothelial heme oxygenase-1 expression: ortho-methoxy groups are essential to enhance heme oxygenase activity and protection (2006) Exp Mol Med 38: 393-400. https://doi.org/10.1038/emm.2006.46
5. Abdel-Daim MM and Abdou RH. Protective Effects of Diallyl Sulfide and Curcumin Separately against Thallium-Induced Toxicity in Rats (2015) Cell J 17: 379-388.
6. Joe B, Vijaykumar M and Lokesh B R. Biological properties of curcumin-cellular and molecular mechanisms of action (2004) Crit Rev Food Sci Nutr 44: 97-111.
7. Wright LE, Frye JB, Gorti B, Timmermann BN and Funk JL. Bioactivity of turmeric-derived curcuminoids and related metabolites in breast cancer (2013) Curr Pharm Des 19: 6218-6225. https://doi.org/10.2174/1381612811319340013
8. Mahady GB, Pendland SL, Yun G and Lu ZZ. Turmeric (Curcuma longa) and curcumin inhibit the growth of Helicobacter pylori, a group 1 carcinogen (2002) Anticancer Res 22: 4179-4181.
9. Reddy RC, Vatsala PG, Keshamouni VG, Padmanaban G and Rangarajan PN. Curcumin for malaria therapy (2005) Biochem Biophys Res Commun 326: 472-474. https://doi.org/10.1016/j.bbrc.2004.11.051
10. Sethi G, Sung B and Aggarwal BB. Nuclear factor-kappaB activation: from bench to bedside (2008) Exp Biol Med (Maywood) 233: 21-31. https://doi.org/10.3181/0707-mr-196
11. Reuter S, Gupta SC, Chaturvedi MM and Aggarwal BB. Oxidative stress, inflammation, and cancer: how are they linked? (2010) Free Radic Biol Med 49: 1603-1616. https://doi.org/10.1016/j.freeradbiomed.2010.09.006
12. Cho JW, Lee KS and Kim CW. Curcumin attenuates the expression of IL-1beta, IL-6, and TNF-alpha as well as cyclin E in TNF-alpha-treated HaCaT cells; NF-kappaB and MAPKs as potential upstream targets (2007) Int J Mol Med 19: 469-474. https://doi.org/10.3892/ijmm.19.3.469
13. Huang CZ, Huang WZ, Zhang G and Tang DL. In vivo study on the effects of curcumin on the expression profiles of anti-tumour genes (VEGF, CyclinD1 and CDK4) in liver of rats injected with DEN (2013) Mol Biol Rep 40: 5825-5831. https://doi.org/10.1007/s11033-013-2688-y
14. Li R, Wang Y, Liu Y, Chen Q, Fu W, et al. Curcumin inhibits transforming growth factor-beta1-induced EMT via PPARgamma pathway, not Smad pathway in renal tubular epithelial cells (2013) PLoS One 8. https://doi.org/10.1371/journal.pone.0058848
15. Anthwal A, Thakur BK, Rawat MS, Rawat DS, Tyagi AK, et al. Synthesis, characterization and in vitro anticancer activity of C-5 curcumin analogues with potential to inhibit TNF-alpha-induced NF-kappaB activation (2014) Biomed Res Int 1–10. https://doi.org/10.1155/2014/524161
16. Nieto CI, Cabildo MP, Cornago MP, Sanz D, Claramunt RM, et al. Fluorination Effects on NOS Inhibitory Activity of Pyrazoles Related to Curcumin (2015) Molecules 20: 15643-15665. https://doi.org/10.3390/molecules200915643
17. Paulino N, Paulino AS, Diniz SN, de Mendonca S, Goncalves ID, et al. Evaluation of the anti-inflammatory action of curcumin analog (DM1): Effect on iNOS and COX-2 gene expression and autophagy pathways (2016) Bioorg Med Chem 24: 1927-1935. https://doi.org/10.1016/j.bmc.2016.03.024
18. de Porras RV, Bystrup S, Martinez-Cardus A, Pluvinet R, Sumoy L, et al. Curcumin mediates oxaliplatin-acquired resistance reversion in colorectal cancer cell lines through modulation of CXC-Chemokine/NF-kappaB signalling pathway (2016) Sci Rep 6. https://doi.org/10.1038/srep24675
19. Pulido-Moran M, Moreno-Fernandez J, Ramirez-Tortosa C and Ramirez-Tortosa C Curcumin and Health (2016) Molecules 21: 264. https://doi.org/10.3390/molecules21030264
20. Pari L, Tewas D and Eckel J. Role of curcumin in health and disease (2008) Arch Physiol Biochem 114: 127-149.
21. Akazawa N, Choi Y, Miyaki A, Tanabe Y, Sugawara J, Ajisaka R and Maeda S. Curcumin ingestion and exercise training improve vascular endothelial function in postmenopausal women (2012) Nutr Res 32: 795-799. https://doi.org/10.1016/j.nutres.2012.09.002
22. Panahi Y, Rahimnia AR, Sharafi M, Alishiri G,Saburi A et al. Curcuminoid treatment for knee osteoarthritis: a randomized double-blind placebo-controlled trial (2014) Phytother Res 28: 1625-1631. https://doi.org/10.1002/ptr.5174
23. Ahn JK, Kim S, Hwang J, Kim J, Lee YS et al. Metabolomic Elucidation of the Effects of Curcumin on Fibroblast-Like Synoviocytes in Rheumatoid Arthritis (2015) PLoS One 10. https://doi.org/10.1371/journal.pone.0145539
24. Lang A, Salomon N, Wu JCY, Kopylov U, Lahat A et al. Curcumin in combination with mesalamine induces remission in patients with mild-to-moderate ulcerative colitis in a randomized controlled trial (2015) Clin Gastroenterol Hepatol 13: 1444-1449. https://doi.org/10.1016/j.cgh.2015.02.019
25. Yu JJ, Pei LB, Zhang Y, Wen ZY and Yang JL. Chronic supplementation of curcumin enhances the efficacy of antidepressants in major depressive disorder: a randomized, double-blind, placebo-controlled pilot study (2015) J Clin Psychopharmacol 35: 406-410. https://doi.org/10.1097/jcp.0000000000000352
26. Rainey-Smith SR, Brown BM, Sohrabi HR, Shah T and Goozee KG. et al. Curcumin and cognition: a randomised, placebo-controlled, double-blind study of community-dwelling older adults (2016) Br J Nutr 115: 2106-2113. https://doi.org/10.1017/S0007114516001203
27. Tenero L, Piazza M, Zanoni L, Bodini A, Peroni D, et al. Antioxidant supplementation and exhaled nitric oxide in children with asthma (2016) Allergy Asthma Proc 37: 8-13.
https://doi.org/10.2500/aap.2016.37.3920
28. Institute of Medicine. Beyond mayalgic encephalomyelitis/chronic fatigue syndrome: redefining an illness (2015) The National Academies Press, Washington DC, United States.
29. Jason LA and Richman JA. How science can stigmatize: The case of chronic fatigue syndrome (2008) J Chronic Fatigue Syndrome 53: 1195–1219.
https://doi.org/10.3109/10573320802092146
30. Twisk FN. The status of and future research into Myalgic Encephalomyelitis and Chronic Fatigue Syndrome: the need of accurate diagnosis, objective assessment and acknowledging biological and clinical subgroups (2014) Front Physiol 5: 109.
https://doi.org/10.3389/fphys.2014.00109
31. Jason L, Sorenson M, Sebally K, Alkazemi D, Lerch A, et al. Increased HDAC in association with decreased plasma cortisol in older adults with chronic fatigue syndrome. (2011) Brain Behav Immun.
32. Morris G, Anderson G, Dean O, Berk M and Galecki P et al. The glutathione system: a new drug target in neuroimmune disorders (2014) Mol Neurobiol 50: 1059-1084.
33. Nijs J, Nees A, Paul L, De Kooning M, Ickmans K. et al. Altered immune response to exercise in patients with chronic fatigue syndrome/myalgic encephalomyelitis: a systematic literature review. Exerc Immunol Rev 20: 94-116.
34. Maes, Bosmans M E and Kubera M. Increased expression of activation antigens on CD8+ T lymphocytes in Myalgic Encephalomyelitis/chronic fatigue syndrome: inverse associations with lowered CD19+ expression and CD4+/CD8+ ratio, but no associations with (auto)immune, leaky gut, oxidative and nitrosative stress biomarkers (2015) Neuro Endocrinol Lett 36: 439-446.
35. Morris G, Berk M, Walder K and Maes M. Central pathways causing fatigue in neuro inflammatory and autoimmune illnesses (2015) BMC Med 13: 28. https://doi.org/10.1186/s12916-014-0259-2
36. Blundell S, Ray KK, Buckland M and White PD. Chronic fatigue syndrome and circulating cytokines: A systematic review (2015) Brain Behav Immun 50: 186-195. https://doi.org/10.1016/j.bbi.2015.07.004
37 van Campen CLMCRKV, F.C. The effect of Curcumin on patients with Chronic Fatigue Syndrome/Myalgic Encephalomyelitis: an open label study (2018) Int J Clinical Medicine 9: 356-366. https://doi.org/10.4236/ijcm.2018.95031
38. Fukuda K, Straus SE, Hickie I, Sharpe MC, Dobbins JG et al. The chronic fatigue syndrome: a comprehensive approach to its definition and study. International Chronic Fatigue Syndrome Study Group (1994) Ann Intern Med 121: 953-959. https://doi.org/10.7326/0003-4819-121-12-199412150-00009
39. Carruthers BM, van de Sande MI, DE Meirleir KL, Klimas NG, Broderick G, et al. Myalgic encephalomyelitis: International Consensus Criteria (2018) J Intern Med 270: 327-338. https://doi.org/10.3390/diagnostics9010001
40. Wagner DR, Nisenbaum C, Heim JF, Jones ER, Unger et al. Psychometric properties of the CDC symptom inventory for assessment of chronic fatigue syndrome (2005) Popul Health Metr 3: 8. http://doi.org/10.1186/1478-7954-3-8
41. Vermeulen RC. Translation and validation of the dutch language version of the CDC symptom inventory for assessment of Chronic Fatigue Syndrome (CFS) (2006) Popul Health Metr 4: 12. http://doi.org/10.1186/1478-7954-4-12
42. Viehoff PB, van Genderen FR and Wittink H. Upper limb lymphedema 27 (ULL27): Dutch translation and validation of an illness-specific health-related quality of life questionnaire for patients with upper limb lymphedema (2008) Lymphology 41: 131-138.
43. Hornig M, Montoya JG, Klimas NG, Levine S, Felsenstein D, et al. Distinct plasma immune signatures in ME/CFS are present early in the course of illness (2015) Sci Adv 1. http://doi.org/10.1126/sciadv.1400121
44. Hornig M, Gottschalk G, Peterson DL, Knox KK, Schultzm AF, et al. Cytokine network analysis of cerebrospinal fluid in myalgic encephalomyelitis/chronic fatigue syndrome (2016) Mol Psychiatry 21: 261-269. http://doi.org/10.1038/mp.2015.29
45. Landi AD, Broadhurst SD, Vernon DL, Tyrrell et al. Reductions in circulating levels of IL-16, IL-7 and VEGF-A in myalgic encephalomyelitis/chronic fatigue syndrome (2016) Cytokine 78: 27-36. http://doi.org/10.1016/j.cyto.2015.11.018
46. Russell L,Broderick G, Taylor R, Fernandes H, Harvey J, et al. Illness progression in chronic fatigue syndrome: a shifting immune baseline (2016)BMC Immunol 17: 3. http://doi.org/10.1186/s12865-016-0142-3
47. Nakatomi Y, Mizuno K, Ishii A, Wada Y, Tanaka M, et al. Neuroinflammation in Patients with Chronic Fatigue Syndrome/Myalgic Encephalomyelitis: An 11C-(R)-PK11195 PET Study (2014) J Nucl Med 55: 945-950. http://dx.doi.org/10.2967/jnumed.113.131045
48. Morris, G., M. Berk, P. Galecki, K. Walder and M. Maes. The neuro-immune pathophysiology of central and peripheral fatigue in systemic immune-inflammatory and neuro-immune diseases (2016) Mol Neurobiol 53: 1195-1219. http://doi.org/10.1007/s12035-015-9090-9
49. Ryu EK, Choe YS, Lee KH, Choi Y and Kim BT. Curcumin and dehydrozingerone derivatives: Synthesis, radiolabeling, and evaluation for beta-amyloid plaque imaging (2006) J Med Chem 49: 6111-6119. http://doi.org/10.1021/jm0607193
50. Chapman KR, Bateman ED, Chen H, Hu H, Fogel R, et al. QVA149 improves lung function, dyspnea, and health status independent of previously prescribed medications and copd severity: a subgroup analysis from the SHINE and ILLUMINATE studies (2015) Chronic Obstr Pulm Dis 2: 48-60. http://doi.org/10.15326/jcopdf.2.1.2014.0140
51. Prasad S, Tyagi AK and Aggarwal BB. Recent developments in delivery, bioavailability, absorption and metabolism of curcumin: The golden pigment from golden spice (2014) Cancer Res Treat 46: 2-18.
http://doi.org/10.4143/crt.2014.46.1.2
52. Cuomo J, Appendino G, Dern AS, Schneider E, McKinnon TP, et al. Comparative absorption of a standardized curcuminoid mixture and its lecithin formulation (2011) J Nat Prod 74: 664-669. http://doi.org/10.1021/np1007262
53. Brown MM and Jason LA. Functioning in individuals with chronic fatigue syndrome: increased impairment with co-occurring multiple chemical sensitivity and fibromyalgia (2007) Dyn Med 6: 9. http://doi.org/10.1186/1476-5918-6-6
Gupta SC, Patchva S and Aggarwal BB. Therapeutic roles of curcumin: lessons learned from clinical trials (2013) AAPS J 15: 195-218. http://doi.org/10.1208/s12248-012-9432-8
54. Gupta SC, Patchva S and Aggarwal BB. Therapeutic roles of curcumin: lessons learned from clinical trials (2013) AAPS J 15: 195-218. http://doi.org/10.1208/s12248-012-9432-8
*Corresponding author
C (Linda) MC van Campen, Department of Cardiology, Stichting Cardiozorg, Hoofddorp, Netherlands, E-mail: info@stichtingcardiozorg.nl
Citation
Campen CMCV and Visser FC. The effect of curcumin in patients with chronic fatigue syndrome/myalgic encephalomyelitis: disparate responses in different disease severities (2019) Pharmacovigil and Pharmacoepi 2: 22-27.
Keywords
Curcumin, Myalgic Encephalomyelitis/Chronic Fatigue Syndrome, Disease severity, CDC score, Fukuda score, R and 36 questionnaire.


 PDF
PDF