Case Summary
We report a 49 year old man who, other than having an unprovoked pulmonary embolism in 2012, is otherwise fit and well. He is originally from Gambia but has been working as a chef in the United Kingdom for the past 25 years. He last travelled to Gambia in 2014, where he spent two weeks. He does not drink alcohol and has never smoked. He has a family history of sickle cell disease, but nil else of note. He presented to hospital in December 2015 with a several week history of malaise, lethargy and shortness of breath. This was associated with a cough which was occasionally productive of clear sputum, and over this period he had a reduced appetite and had lost half a stone in weight. On examination he was cachectic and had bilateral cervical lymphadenopathy. He reduced bi-basilar air entry on his chest and abdominal examination revealed hepatomegaly. Cardiovascular examination was unremarkable, with no evidence of a murmur or pericardial knock. He had no signs of clubbing or peripheral oedema. No skin rashes were noted. Bedside observations were stable other than tachycardia (112 Beats per Minute (bpm)); of note, blood pressure was normal. His initial investigations showed chronic microcytic anaemia with a Mean Corpuscular Volume (MCV) of 71 fl. He had raised inflammatory markers with C-Reactive Protein (CRP) of 73mg/L and Erythrocyte Sedimentation Rate (ESR) of 15 mm/hr. Sputum cultures including those for Acid-Fast Bacilli (AFB) were negative. Chest X-ray demonstrated bilateral pleural effusions with bi-basal consolidation.
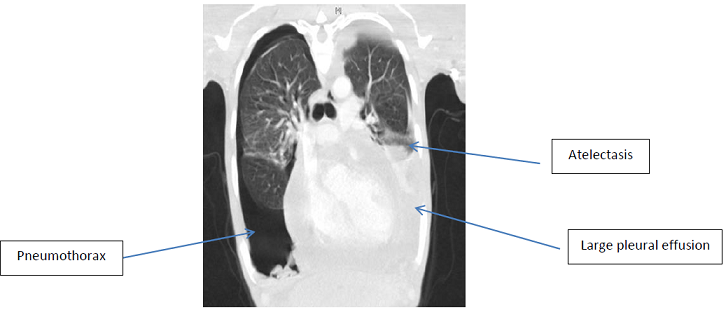
Further investigation including a Computer Tomography (CT) of his chest revealed enlarged axillary, cervical and supraclavicular lymph nodes as well as pericardial and bilateral pleural effusions with a right sided pneumothorax. He then went on to have an echocardiogram which showed moderate circumferential pericardial effusion with fibrinous strands; his ejection fraction was 64%. There were no echocardiographic features of tamponade at that point, although he had septal bounce and Tissue Doppler Imaging (TDI) patterns across the mitral and tricuspid inflows were consistent with a constrictive effusive picture. Intravenous Cholangiogram (IVC) at this time was <2 cm and collapsed ~ 50%, which represents normal filling pressures. The main differential diagnosis at this stage was pulmonary tuberculosis complicated by pleural and pericardial effusions and a pneumothorax. Upon review by the respiratory team, he was started on the full anti-tuberculosis treatment as well as 60mg of prednisolone (equivalent to 30mg due to Rifampicin interactions) for the pericardial involvement. His left pleural effusion was drained for symptomatic relief. The pleural fluid was exudative and lymphocytic with a protein of 55.3 g/L, LDH of 178 u/L and few White Blood Cells (WBC), 95% of which were lymphocytes. The fluid glucose was 6.3 mmol/L. An incision biopsy of his left axillary lymph node was performed, which revealed reactive lymphadenitis. pleural fluid, serial sputum and lymph node fluid cultures were, however, negative for TB (Figure 1).
He was discharged from hospital when his symptoms had improved with a plan to continue TB quadruple therapy and a weaning regime of steroids (10 mg every 5 days). At subsequent outpatient appointments in the TB clinic, he was noted to be making good recovery. He started gaining weight and appetite returned to normal. His pleural and pericardial effusions also improved and this reflected in improvement in his cough and breathing. His cervical and supraclavicular nodes had also shrunk in repeat imaging. Six weeks into his anti-TB treatment when he was on 10mg prednisolone, his symptoms relapsed and he developed further anorexia, weight loss and fatigue. At this stage he also experienced significant shortness of breath on minimal exertion and orthopnea. He was thereafter reviewed in the cardiology clinic as an outpatient and was noted to be short of breath at rest (Respiratory Rate (RR)-24) and remained tachycardic (120bpm) but normotensive with a positive Kussmauls sign, suggesting limited right ventricular filling. An immediate trans-thoracic echocardiogram was performed which showed a recurrence of his pericardial effusion (1.5 cm globally) with semi-fibrinous material and progression of his constrictive physiology.
As well as the septal bounce and TDI patterns seen on the first echocardiogram, there was now a dilated inferior vena at 3.3 cm cava with flow reversal into the hepatic veins on color doppler imaging. The Left Ventricle (LV) remained non-dilated and Ejection Fraction (EF) was preserved. The constrictive picture was later confirmed with cardiac Magnetic Resonance Imaging (cMRI) which demonstrated circumferential thickening of the pericardium (13 mm) with features of inflammation and constriction associated with a small pericardial effusion and normal myocardium. The inferior vena cava and hepatic veins were severely dilated. The left and right ventricles were noted to be small and he had an LV EF of 70% on cMRI (Figure 2).
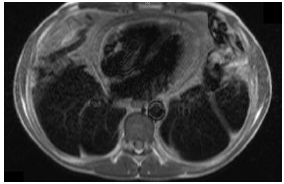
Due to a clinical relapse despite an extensive course of anti-TB treatment, diagnosis was reconsidered with further differentials such as chronic infection (toxoplasma, fungal, parasitic), haematological malignancy and systemic autoimmune diseases and investigations performed accordingly. The prednisolone dose was increased back to 50mg daily. TB treatment continued as diagnostic uncertainty at that time, and the concern that if TB were a co-factor then flare of this disease with immunosuppression may be potentially serious. Toxoplasma, schistosoma and mycoplasma serology was negative and haematological malignancy was unlikely based on the prior lymph node biopsy result. Malignancy markers (AFP, CA125, CA19, CEA, HCG and PSA) were negative, and anti-IgG4 level was normal. The autoimmune screen, however, revealed a positive Anti-Nuclear Antibody (ANA) of 1:640 with a fine speckled pattern, positive anti-dsDNA with a titer of 30, positive anti-Smith antibody and normal C3 and C4 levels. His urine analysis showed trace of blood, and significantly raised urine protein: creatinine ratio at 177 mg/mmol. In keeping with the American College of Rheumatology (ACR) diagnostic criteria, Systemic Lupus Erythematosus (SLE) was then diagnosed based on the presence of pericarditis, proteinuria, positive ANA and anti-dsDNA Ab. The prednisolone dose was increased to 60 mg (30 mg equivalent due to Rifampicin) and hydroxychloroquine was initiated. Upon discussion with Cardiology, 0.5 mg colchicine twice daily was also started for symptomatic relief of constrictive pericarditis. After months of treatment, his fatigue and systemic symptoms had improved, but he remained symptomatic from constrictive effusive pericarditis, with ongoing symptoms and signs of right sided heart failure.
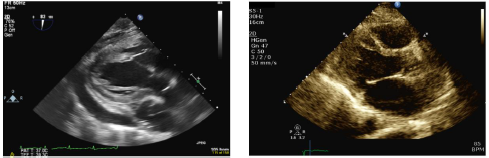
A subsequent uncomplicated pericardiectomy was performed, which resulted in a complete resolution of the signs of right sided heat failure and shortness of breath. Pericardial biopsy results showed granulomatous inflammation and fibrosis; TB cultures were negative. A subsequent renal biopsy showed features of membranous lupus nephritis. A repeat echocardiogram following the procedure showed mild septal bounce with no effusion but preserved biventricular function and normal sized ventricles, consistent with a significant resolution of his constrictive physiology post pericardiectomy (Figure 3).
Discussion
To the best of our knowledge, only six cases of systemic lupus erythematosus with constrictive pericarditis have been reported in English literature. Of these, four patients were male and two female, with a median age of 38 years (range 17-58 years). Only two patients had a prior diagnosis of SLE and TB was part of the differential diagnosis in at least five cases. The progression from exudative pericarditis to constrictive pericarditis ranged from one week to six months and some authors postulated that it might have been triggered by rapid reduction of prednisolone dose. Only one of these six cases had an effusive-constrictive pericarditis similar to our case. The diagnosis of constrictive pericarditis was confirmed by echocardiography, right ventricular catheterization or cardiac MRI (Table 1) [1-7].
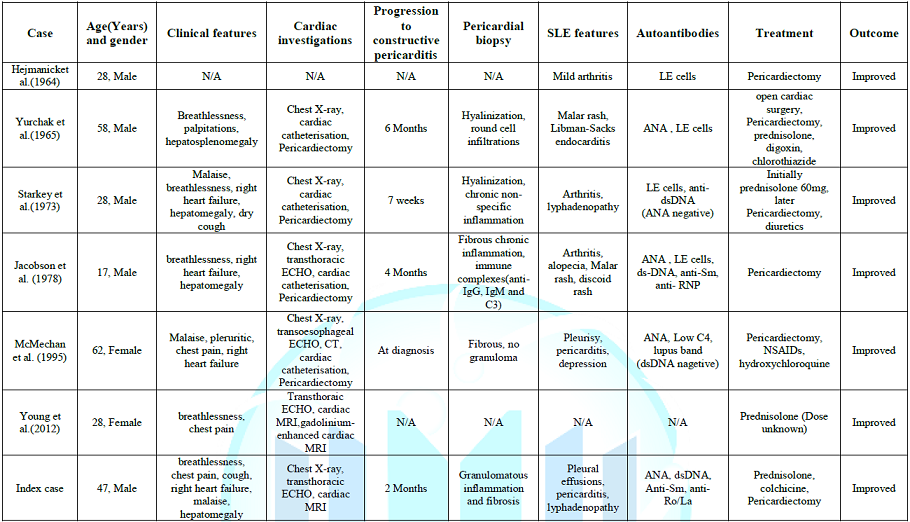
Five of six patients underwent pericardiectomy and pericardial biopsy reports were described in four cases. Overall, the histopathological findings were non-specific: two biopsies showed hyalinization and either round-cell infiltration or non-specific inflammation, other two demonstrated fibrosis with inflammation but no granulomas [2,4-6]. Immunohistochemistry was performed in the case described by Jacobson et al. [2] and it revealed the presence of anti-IgG, IgM and C3 in pericardial tissue. Our patient is the only case that demonstrated granulomatous inflammation and fibrosis; still the TB cultures were negative. Cardiac symptoms resolved with steroid treatment alone in only one case; in five patients, as well as in our patient, pericardiectomy was performed leading to symptoms resolution [3]. All patients survived.
Conclusion
Although the most common causes of constrictive pericarditis are infectious or idiopathic, this case highlights that underlying connective tissue diseases should also be considered as a differential diagnosis, especially in those cases with no proven etiology and without improvement with antimicrobial or antiviral treatment. Although constrictive pericarditis is a rare feature in SLE, a high index of suspicion is needed in patients who have worsening shortness of breath despite a normal initial echocardiogram. In such cases, a Cardiology opinion and cardiac MRI may be of value in identifying underlying complications. Although it is difficult to make conclusions regarding gender prevalence when only seven cases have been reported we note that five (71%) of these patients were male; it is well-known that SLE has a female preponderance though male patients with SLE often have more severe disease, which may account for the higher proportion of male patients with constrictive pericarditis in our literature review. In such patients with constrictive pericarditis, even though corticosteroid treatment may partially alleviate the symptoms a Pericardiectomy is likely to be required for definitive treatment. While a pericardial biopsy might reveal non-specific features of acute or chronic inflammation, it should be performed in all cases if possible, in order to exclude underlying infection.
References
2. Jacobson EJ and Reza MJ. Constrictive pericarditis in systemic lupus erythematosus. Demonstration of immunoglobulins in the pericardium (1978) Arthritis Rheum 21: 972-974. https://doi.org/10.1002/art.1780210815
3. Young Oh J, Chang SA, Choe HY and Kim DK. Transient constrictive pericarditis in systemic lupus erythematosus (2012) European Heart J Cardiovascular Imaging 13: 793. https://doi.org/10.1093/ehjci/jes052
4. Yurchak PM, Levine SA and Gorlin R. Constrictive pericarditis complicating disseminated lupus erythematosus (1965) Circulation 31: 113-118. https://doi.org/10.1161/01.CIR.31.1.113
5. Starkey RH and Hahn BH. Rapid development of constrictive pericarditis in a patient with systemic lupus erythematosus (1973) Chest 63:448-450. https://doi.org/10.1378/chest.63.3.448
6. Mcmechan SR, McClements BM, McKeown PP, Webb SW and Adgey AA. Systemic lupus erythematosus presenting as effuso-constrictive pericarditis (1995) Postgraduate Medical J 71: 627-629. https://doi.org/10.1136/pgmj.71.840.627
7. Hejmancik MR, Wright JC and Quint R. The cardiovascular manifestations of systemic lupus erythematosus (1964) American Heart J 68: 119-130. https://doi.org/10.1016/0002-8703(64)90248-0
*Corresponding author
Hannah Jethwa, Department of Rheumatology, Addenbrookes Hospital, Cambridge, United Kingdom, Tel: +01223 217457 E-mail: hannahjethwa@nhs.net
Citation
Jethwa H, Rana M, Kitt J, Menzies S, Steuer A, et al. Constrictive pericarditis as the first presentation of systemic lupus erythematosus (2019) Rheumatic Dis Treatment J 1: 10-12.
Keywords
Lupus, Autoimmune disease, Bilateral cervical lymphadenopathy,Cardiovascular examination.


 PDF
PDF