Research Article :
Background: Rural nursing practice and education remain a
difficult task to achieve in first world countries, let alone in a third world
country like Lebanon. The latter sustained 15 years of civil war, followed by
ongoing political and economic instability. North and South Lebanon, and Bekaa
are rural sites, and are considered the most socioeconomically-disadvantaged
geographic locations in the country. This includes severe shortage in Nursing
practice and education. Purpose: The aim of this study is to share the experience in
the provisional establishment of a School of Nursing in rural Lebanon, hoping
that such an initiative would help in lessening the severity in the shortage of
qualified nurses rurally, and, thus, in improving health care. Method: The model followed is based on four main pillars,
namely approaching the locals, establishing the matrix, designing the
curriculum, and setting-up research priorities. Each of these pillars consists
of various components at different levels. Results: Approaching the locals and establishing the matrix
are essentials and prerequisites for the other two main pillars. The former is
time-consuming, requires well-trained human resources, and takes a big
proportion of the time allocated to the project. Establishing the matrix,
designing the curriculum, and setting-up research priorities are
equally-important, and each has its own peculiarities and requirements that are
summarized in this manuscript. Setting-up a rural School of Nursing in Lebanon is not a privilege. It
is rather a necessity, and requires careful planning and allocation of
significant human and non-human resources. However, the experience is very much
enjoyable, has a unique flavor, and provides the best solution for the severe
shortage in qualified nurses from which the local villages suffer. Lebanon
is a small country with a landscape not exceeding 10,452 km2, and
with a population of 6,229,794 based on the 2017 statistics [1]. The urban
population accounts for 88.6% of total population [1]. Torn with political
instability, the country went through 15 years of civil war, followed by
ongoing socioeconomic hardships resulting in low income, high unemployment
rate, and poverty. Such indicators are even more pronounced in the rural
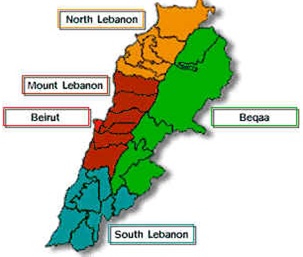
governorates or provinces (also called Mohafazats), namely North Lebanon, South
Lebanon, and Bekaa [2] (Figure 1). Figure 1: Map of Lebanon showing the various districts
(mohafazats or governorates). The
first post war official report on poverty, growth and income distribution in
Lebanon was published by the United Nations Development Programme (UNDP) in
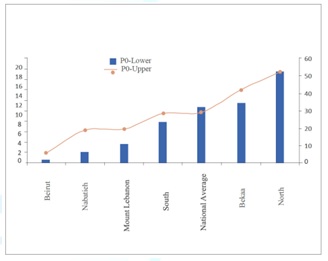
2008 [2]. The results showed an above average prevalence of extreme poverty in
Bekaa and the South (10-12%), an average prevalence of overall poverty in Bekaa
(29%), and an above average
prevalence of overall poverty in the South (42%). A very high prevalence of
extreme and overall poverty in the North (18% and 53%, respectively) was
reported [2] (Figure 2). The
UNDP report also showed that there is a lower likelihood of school and
university enrolment, attendance and retention for the poor residing in these rural
areas of Lebanon [2]. The gaps between poor and non-poor in enrollment
rates were found to widen from elementary to intermediate, secondary, and
tertiary education. Only one poor child out
of two is enrolled in intermediate schools, and only one poor child out of four
is enrolled in secondary schools [2]. The ratio becomes even worse in tertiary
education enrollment. The corresponding ratios for the non-poor are three
out of four for intermediate schools, and one out of two for secondary education.
Therefore, education seems to highly correlate with poverty in Lebanon, whereby
almost 15% of the poor population is illiterate, as compared to only 7.5% among
the non-poor. The unemployment
rate in the non-poor cohort is half the rate seen in the poor one.
Moreover, even if poor citizens were able to break the vicious circle of
education and poverty, and they were able to complete their education, they
could not enter the job market as easily as the non-poor ones.
The
health care services in rural Lebanon seem to follow the same above-mentioned
education and poverty trend [3]. According to the Planning Unit at the Lebanese
Ministry of Public Health, there are approximately 3,000 beds in the public
sector and 12,000 in the private one. Some of the former are not active,
which decreases the percent supply of active beds from the public sector [3].
Private hospitals do not deliver the same quality of services to the rich and
poor. The majority of private hospitals are general and multidisciplinary with
less
than 100-bed capacity. Traditional public hospitals are rather small
with
the largest ones having 70 active beds [3]. In addition, they are poorly
equipped and lack qualified personnel, namely registered nurses (RNs) holding a
Bachelor of Science in Nursing (BSN) degree. Lebanon continues to suffer from
a severe shortage in nurses in general, and RNs in particular. The ratio of
qualified nurses to 1000 population was 0.625 in 2002, 1.786 in 2007, and 2.562
in 2014, thus continues to be one of the lowest in the world [4,5]. The shortage
results from several reasons, including the unattractive professional status
(stigma), being mainly a female career, and a high turnover. Another major
reason for the severe shortage of nurses in the rural areas of Lebanon is the
low number in the Schools
of Nursing offering a BSN degree in these areas, as well as the poverty
described earlier, which limits the high school graduates from enrolling in
such degrees [2-5]. According to latest statistics released by the Order of
Nurses in Lebanon, the total number of nurses registered with the Order up
until the end of December 2017 was 15,034, of which 79.7% are females and 20.3%
are males [6]. The majority of the nurses are aged between 26 and 45. The ones
who are still in the workforce accounted for 73.4%, and those who hold a BSN
degree accounted for 50.1% only. The distribution of these nurses in rural
Lebanon was 14.7% in the North, 9.3% in Bekaa, and 14% in the South. The
majority (84.6%) of these nurses work in hospitals, a very small percentage
(4.7%) in medical centers (primary care, clinic, infirmary, public health
outlet, dispensary, midwifery,
maternity, rural
health), and even a smaller percentage (1.4%) in schools or nurseries
[6]. South Lebanon consists mainly of agricultural
villages and communities, with the major local towns being Saida, Tyre, and
Nabatieh (Figue 3). It has a
population of 816,541 inhabitants, and an area of 1988 km² [1]. Based on the
situation analysis summarized in this introduction, and as an attempt to meet
the needs of the local communities in South Lebanon, Phoenicia University was
established in the District of Zahrany, south of the Litani river. Its main
goal is to provide quality
tertiary education at an affordable fee, be it for the residents of this
rural governorate (province) or for any student residing in the other rural
governorates (provinces) in Lebanon. Since serving the community is among the
vision and mission of the university, and based on the severe shortage in
qualified RNs in South Lebanon, a decision was recently taken by the university
to plan a School of Nursing with a unique program that is
community-based-rural-health-oriented. This paper summarizes this plan, and
could be used as a platform for planning other rural Schools of Nursing in the
outback. Figure 3: Map of Lebanon
listing the various cities and towns. ArabiaGIS 2008. Planning a Rural
School of Nursing
This section summarizes the
process followed in the provisional establishment of a rural School of Nursing
at Phoenicia University. The model we followed consists of four main pillars,
each containing various components at various levels. Approaching
the Locals
Rural communities differ from the
urban ones, and so do the facilities available [7]. Understanding the culture,
tradition, and mentality of the rural communities are the key to any successful
project to be launched in the area, let alone establishing a university degree
in Nursing [8-12]. Such an understanding is only achieved by meeting the
individuals and their extended families, the farmers, the school principals and
teachers, the educated and uneducated
residents, the chiefs of the villages who are often the presidents of both
the villages municipalities and their extended families, the directors and
senior staff of the local
hospitals and medical centers, the financial sector, and the religious
leaders (priests and sheikhs). Such meetings provide a valuable insight, and
help in feeding a multilevel database in relation to what the local health care
needs are, disease prevalence, and how the new degree program could be designed
to help in meeting those needs. As such, they abet in validating the professional
and academic relevance, the continuous need for the Nursing
program, the feasibility for a new School of Nursing, the financial
liability and viability (how much of the income, expenditures and share of
resources that the Nursing program has could affect room for expansion and
program stability, and endowments and financial aid programs for students,
including scholarships, loans and grants), and the available overall resources.
The meetings also help in setting up the context within which the Nursing
program will exist, positioning the goals, categorizing the curriculum content,
framing the curriculum, forecasting for instruction, and structuring
evaluation.
Establishing
the Skeleton Matrix Having
identified the needs of the local communities in South Lebanon, a matrix is set
up to align those needs with the appropriate skeletons [8-12]. The latter
include the parent institution and its philosophy and mission in relation to
education, service and research/scholarship. They also include the physical
space and infrastructure on campus to be allocated for the new degree program,
such as lecture halls, laboratories, simulation and virtual
clinic facilities, library and student services, academic services, and
instructional technology support (distance education resources). The
potential faculty and student characteristics, the economic situation and its
impact on the curriculum, and a comprehensive outline of the health care system
to maintain the curriculum are other skeletons to focus on. In addition,
commuting of students, faculty and support staff is an essential skeleton to
carefully consider. Other major skeletons include partnership of the degree
program with the primary, secondary, and tertiary
health care facilities available in the region, be it government
institutions or private ones. These facilities will serve as clinical attachment
(clerkship, practicum) sites for the potential nursing students, and, as such,
will play a vital role in ensuring that the students have developed the
competencies required to safely practice the profession upon graduation.
Another
important skeleton is the demographic information gathered during the
above-mentioned meetings, such as age, sex, education levels, language (Arabic,
French, and English), socioeconomic status, etc. This information helps in
identifying potential students and their characteristics, the demands of the
population that the graduates will serve, and the nature of the curriculum to
be designed (adult versus young learning theories and modalities). For
instance, the current shortage in RNs holding a BSN degree indicates the possibility
for an accelerated program, and the current shortages in nursing specialties
necessitate advanced
practice curricula which provide the RNs with opportunities for continuing
education. This demographic information also helps in identifying existing and potential
part-time and full-time faculty, adjunct faculty, clinical instructors, and
clinical preceptors, and how their research
and educational credentials compare to others. Still another important
skeleton is benchmarking. This is to compare the program against those offered
by other Schools of Nursing nationwide, regionally, and internationally.
Comparison indicators to be used include pass rate on the Lebanese Nursing
National Licensing Exam or Colloquium, accreditation, graduate employment
rates, national and international reputation, admission and retention rates,
and costs of the program, to name a few.
Establishing
an Advisory Board for the new program is an essential skeleton too. Members of
the Board should include the Dean or Director of the Program, the Chancellor,
the President of the university, a representative from the Board of Trustees,
the President of the Order of Nurses in Lebanon, representatives from both the
Lebanese Ministries of Public
Health and Higher Education, senior officials from international (North
American, Australian, European) Schools of Nursing, directors of the local
public and private hospitals and medical centers, and representatives from the
student body, faculty, community, and major businesses in the region. Detailed
policies and procedures for the whole program is written and revised, and an
analysis of the structure of the parent institution and that of the Nursing
program is set in place to describe the hierarchal and formal lines of
communication. Various levels of steering committees and subcommittees,
including Nursing curriculum committee, college curriculum committee, and
university curriculum committee are set in place as well.
The
Curriculum
The
proposed curriculum is a community-based-rural-health-oriented
one [11,12]. It consists of nine intensive semesters (fall, spring, and
summer), and is based on credit hours. Content delivery will be through
Problem-Based Learning (PBL), Team-Based Learning (TBL), Evidence-Based Nursing
(EBN), didactic lectures, practical laboratory sessions, simulation sessions,
and bed-side teaching through clinical rotations in primary, secondary, and tertiary
health care settings. Basic, clinical, and human
sciences will be integrated vertically and horizontally throughout the
curriculum. In addition to the generic health topics often taught in a BSN
degree, emphasis will be on the common diseases and disorders identified in the
visited communities and in the epidemiological health indicator database,
including incidence, prevalence, birth and death rates, maternal and infant
mortality rates, risk factors, occupation, etc. Formative and summative
assessments will be used at all time, and a competency checklist, a logbook,
and a portfolio focusing on knowledge, clinical skills, attitude, ethics, communication
skills, research, and professional development will be accompanying the
students from day one. External examiners will be invited at the end of each
semester, and will act as both independent examiners of the students and
evaluators of the program. Throughout the curriculum, each learning activity
will be linked to a quick and short online evaluation form to be filled in by
the students. All the teaching staff will also fill in a short and quick online
feedback form, which the students could access to monitor their academic
performance. A faculty-student retreat will be conducted at the end of each
academic year to reflect on both the contents and processes pertaining to the
curriculum and degree program. Rural
Health Nursing Research
Integration
of rural health nursing research in our curriculum is paramount. This is based
on the fact that bridging scholarship and research in Nursing could evolve into
evidence-based Nursing practice [13-16]. In fact, such bridging could cross all
disciplines, and could lead to interprofessional collaboration and
evidence-based practice, based on the newest breakthroughs and research in
health care Nursing and education. It plays an increasingly important role in
its contributions to Nursing
practice, specifically to the professional postgraduate degrees in Nursing
(MSN, DNP, PhDN). Again, the initial community visits described earlier provide
a realistic database in both listing and prioritizing research topics in nursing
to be integrated into the curriculum. This is based on the fact that
partnerships between community members and academic investigators are essential
to the success of human studies in rural communities. For instance, research to
explore the holistic impact of a rural health problem depends on questions
queried by community members living with the direct physical, spiritual,
social, emotional, and/or economic effects of exposure. The research topics
added to our database include costs of hospital admission and stay, medications
and doctor consultations. They also include pre-marriage counseling, womens
health, mental health, mens health, occupational health and job security,
general health care ease-of-access and remoteness for the elderlies, oral
health, village health and wellbeing, primary care, rural ageing, nutrition,
child health and wellbeing, rural
health education and service delivery, cultural and social aspects of rural
health, accidents and emergency, and chronic diseases and palliative care. Studies have shown that no matter
what the incentives are in recruiting qualified nurses to rural regions, the
best solution remains to establish a Nursing
degree program in these regions, and to recruit Nursing students from the
locals [17]. This ensures that an optimal number of qualified nurses will be
retained to serve the rural disadvantaged communities from which these nurses
originate.
We summarized in this manuscript
a model for establishing a BSN degree in rural Lebanon. The model is based on
four pillars, each containing various components that need to be addressed
thoroughly and at different levels. We follow at Phoenicia University a motto
that states that “leaders are not born, they are crafted”. Such a motto
summarizes our universitys overall philosophy, vision, and mission. It has been
translated in many shapes and forms by the university since its inception, the
latest being the decision to establish a unique rural School of Nursing in
Lebanon. The challenges are many, especially with the poor
economy and health care system from which the whole country has been
suffering for years, let alone the rural areas. However, the university
believes that it has an obligation to serve the rural communities all over
Lebanon, and that when there is a will there is a way.
1. World population prospects: The
2017 revision (2017) Department of economic and social affairs, Population division
volume II: Demographic profiles, UN, New York, USA. 2.
Laithy HE, Abu-Ismail K and
Hamdan K. Poverty, growth and income distribution in Lebanon (2008) United
Nations Development Programme (UNDP), UN, New York, USA. 3.
Health systems profile (2006)
Regional Health Systems Observatory- EMRO, Lebanon. 4.
Ammar W. Health system and reform
in Lebanon (2003) WHO, Beirut, Lebanon. 5.
Density of nursing and midwifery
personnel (total number per 1000 population) (2018) WHO Global Health
Observatory. 6.
Order of nurses in Lebanon (2017),
Lebanon. 7.
Spoont M, Greer N, Su J, Fitzgerald
P, Rutks I, et al. Rural vs. Urban ambulatory health care: A systematic review
(2013) CreateSpace independent publishing platform, Washington DC, USA. 8.
Johnson M. Intentionality in
education (1977) Lebanon. 9.
Lohmann A and Schoelkopf L. GIS -
A useful tool for community assessment (2009) J Prev Interv Comm 37: 1-4. https://doi.org/10.1080/10852350802498326 10. Walker A, Bezyak J, Gilbert E and
Trice A. A needs assessment to develop community partnerships: Initial steps
working with a major agricultural community (2011) Am J Health Ed 42: 270-275. https://doi.org/10.1080/19325037.2011.10599197 11. Charlene
AW and Helen J Lee. Rural nursing: Concepts, theory, and practice 4th
edn (2018) Springer publishing company LLC, New York, USA. 12. Sarah
BK. Curriculum development and evaluation in nursing 3rd edn (2014) Springer
publishing company LLC, New York, USA. 13. Aduddell
KA, and Dorman GE. The development of the next generation of nurse leaders
(2010) J Nurs Ed 49: 168-171. https://doi.org/10.3928/01484834-20090916-08 14. Evans
N, Michelle L and Komla T. A systematic review of rural development research:
characteristics, design quality and engagement with sustainability (2015)
Springer International Publishing, New York, USA. 15. Anderson
CA. Current strengths and limitations of doctoral education in nursing: Are we
prepared for the future? (2000) J Prof Nurs 16: 191-200. https://doi.org/10.1053/jpnu.2000.7830 16. Udlis
KA and Manusco JM. Doctor of nursing practice programs across the United
States: A benchmark of information. Part I: Program characteristics (2012) J
Prof Nurs 28: 265-273. https://doi.org/10.1016/j.profnurs.2012.01.003 17.
Gisèle M, Gagnon MP, Paré G and
José C. Interventions for supporting nurse retention in rural and remote areas:
An umbrella reviews (2013) Hum Res Health 11: 44. https://doi.org/10.1186/1478-4491-11-44
Establishing a Rural School of Nursing in Lebanon: A Practical Model
Abstract
Full-Text
Background

Method
Discussion and
Conclusion
References