Review Article :
Abstract Objective: To evaluate the impact of soft tissue factors in dental implants. Data: Studies evaluating the role of soft tissues in dental implants were included in this review. Sources: A comprehensive literature search of English and Chinese language articles was performed via electronic databases (PubMed, Cochrane Library, Web of Science, CNKI and VIP) using the appropriate key words(esthetic; evaluation; impact factor; soft tissue). The most recent search took place in January 2016. Study selection: Potentially appropriate articles were identified and evaluated for eligibility through a predefined review process conducted by two examiners. Only 16 out of the 346 identified records met criteria and were included in the final analysis. Conclusion: The success of dental implants depends on two outcomes, the functional utility of the implant and its beauty. During the early phase of treatment, the main objective of a dental implant is to achieve adequate function. In clinical practice, however, subsequent soft tissue retraction and implant exposure have a significantly negative impact on implant esthetics, especially in young women’s teeth, which can also be considered as implant failure. It is particularly important to understand how to support the surrounding soft tissue so that it is esthetically pleasing.
The Pink Esthetic Score
(PES) is a simple yet complete tool for assessment of esthetic parameters [1].
The PES is a composite score of the tooth volume/outline [2], mesio-gingival papilla,
distal gingival papilla, labial margin curvature, labial edge height, and the
color and texture of soft tissue. How does one categorize the gingival papilla level? Gingival
papilla level 0: no gingival papilla; level 1: gingival papilla < ½ teeth gap; level II:
gingival papilla > ½ teeth gap; level III: gingival papilla is full of teeth
gap; level IV: gingival papilla overgrowth teeth gap. Gingival biotype is the thickness of
the gingiva in the faciopalatal dimension
[3]. Generally, the biological types of gums are divided into 2 types: thin and
thick gingival biotype. It is defined thick gingival biotype when the thickness
of the buccal mucosa is larger than or equal to 1.5 mm. It is defined thin
gingival biotype when the thickness of the buccal mucosa is less than 1.5 mm.
Probe visibility is the clinical gold standard to discriminate thick biotypes
from thin ones, but this method is prone to subjective interpretation. It has a
significant impact on the outcome of restorative, regenerative implant therapy.
Biotype is one of the critical factors that determine the result of dental
treatment. Initial gingival
thickness predicts the outcome of any root coverage procedures or any
restorative treatments. Compared with thin gingival biotype, thick ones have
obvious advantages in preventing the withdrawal of fibrous tissue and bone
tissue [4], because there is the support of more blood supply. The distance between supracrestal soft tissue attachment of periodontal tissue and
the tooth/root surface has been termed biologic width [5], an important concept
in periodontics and
restorative dentistry.
Both attached epithelial cells and connective tissue attachment complex make
important contributions to periodontal health during prosthetic treatments,
since invading this zone can cause bone resorption and gingival recession. The
concept is introduced into the field of implantation. Implant biologic
width is the distance established by “the junctional epithelium
and connective tissue attachment to the implant surface”. In
other words, it is the height between the deepest point of the gingival sulcus and
the alveolar bone crest.
This kind of natural enclosure can provide isolation from the oral environment
and protection for peri-implant bone tissue in order to maintain the stability
of implants. The mean biologic width was determined to be 2.04 mm, of
which 1.07 mm is occupied by the connective tissue attachment and
another approximate 0.97 mm is occupied by the junctional epithelium
[6,7]. The thicker biotype of the gingival mucosa has
the more enough space to support biologic width. In other words, during dental
restoration in a patient with thick biotype gingival mucosa, it is more
difficult to infringe upon the biologic width. An esthetic outcome is much more
likely gained in thick biotype gingival mucosa. Esthetic effect obtained in the labial gingiva [8] is
closely related to labial lateral bone wall thickness. Thickness greater than
2mm gives greater certainty of aesthetic effect and implant stability. The long-term success of restorative implants is based upon
the thickness of bone surrounding the implants,
[9] especially the bone between two implants. The ideal lateral space between
implants and tooth is 3 to 4 mm. Gastaldo [10] found that it is difficult to
form gingival papilla when the distance between implant edges or the horizontal
distance between adjacent teeth is less than 3mm. The inter-implant distance
should not be less than 3mm and the distance between the natural teeth and
implants should be at least 1.5mm in order to ensure that the peri-implant is
surrounded by the integrity of alveolar bone. CPB is the distance between the crown contact point of the
teeth and the crest of bone [11]. CPB less than or equal to 5 mm results in an
ideal esthetic effect. If CPB is less than or equal to 4 mm, gingival papilla
recovery is 100%; if CPB is greater than 4 mm but less than or equal to 5 mm,
average gingival papilla recovery is up to 88%; if CPB is greater than 5 mm,
gingival papilla recovery is less than 50%. In addition, some scholars believe
that in maxillary anterior teeth area single tooth implant restoration,
controlling CPB to less than or equal to 4 mm, can avoid the “black triangle”. A wider distance between implants corresponds with a lower
CPB, the teeth gap can be filled with gingival papilla more easily. In other
words, when considering the distance between implants, one should
take into account the CPB. Otherwise, it may be difficult to fill the gap
between the dental implants and therefore difficult to guarantee an esthetic
outcome. Keratinized gums
around the natural tooth and implant play several important roles, including:
withstanding mechanical friction and avulsion, counteracting adjacent tension
of the fraenum linguae, stabilizing the gingival margin, preventing plaque
retention and buffering the biological forces from the mucous membrane of
muscle fibers. Therefore, the contribution of a proper Keratinized mucosa width
is to maintain the healthy defense mechanism of tissues surrounding the
implants. Lang’s [12] study of the relationship between gingival and periodontal health
proposed that in order to maintain healthy gums, one must have a 2mm wide
keratinized gum, including 1 mm of free gingiva and 1 mm of attached gingiva.
When KMW was greater than 2 mm, there was no detectable plaque or gum inflammation on
the tooth surface. When KMW was less than 2 mm, there was obvious gingival
recession. This positive effect of the gums surrounding the implant leads to a
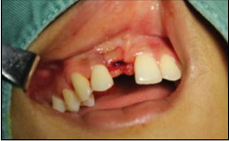
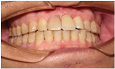
considerably better esthetic effect. Figure 1: After dental implant. Figure 3: After tooth restoration. Periodontitis in adjacent teeth can affect esthetics [13],
whereby resulting in alveolar bone resorption, which may lead to reduced or
absent papilla between implants. In addition, implant failure may occur due to
coexistent inflammation in the root apex, which can affect the adjacent bone
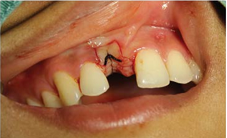
tissue within 1 cm of the root apex [14,15]. The role of surgical suture is to
maintain tension in the wounds and promote the healing. Ideally, sutures should
have a certain tensile strength and a stable absorption rate, at the same time
histologic reaction is mild and
predictable. Dental Implants [16] are today considered as a reliable
treatment option to replace missing teeth both for esthetics and function. The
success of an implant restoration depends on proper implant placement and the
hard and soft tissue architecture that surrounds the fixture and its gums,
shape, color and texture is coordinated with adjacent teeth that close to the
state of the nature. The gingival papilla exists or not and its shape are
important factors that effect on the aesthetic of implant denture, but it has
certain limitations to recover the loss of gingival papilla and easy to be
ignored, so the implant denture gingival papilla aesthetic problems have
gradually become the current focus of the field of dental implants. The aesthetic effect of the gingival papilla is still the
bottleneck in implant denture restoration at present, but the aesthetic effect
can be predicted according to anatomy of adjacent edentulous space, it is
conducive for the physicians and patients to choose treatment scheme in order
to achieve aesthetic and functional results. In addition, healthy keratinized
gingiva is an important factor to ensure the aesthetic effect of dental implant restoration,
especially in the anterior and premolar area. In order to obtain long-term stable aesthetic restoration,
ensure the health of soft tissue and coordinate with the surrounding tissue,
the transplantation of soft tissue technology, appropriate healing cap and a
temporary soft tissue remodeling can be used when soft tissue is not adequate. The reconstruction of the soft
tissue surround the implant denture is to provide a stability of the gingival
structure. Because stable soft tissue surround the implant denture can provide
a close and mechanical defence to prevent bacterial invasion and
improve long-term success rate. In order to obtain satisfactory and aesthetic restoration,
we should improve the implantation plan to repair the factors that affect the
aesthetics of the implant
denture by layer analysis and processing. BW: Biologic width CPB: The distance between alveolar ridge
crest to Crown Point of contact KMW: Keratinized mucosa width Conflicts of Interest The author declares that he has no
conflicts of interest. 1. Perelli M, Abundo
R, Corrente G, Saccone C, Zambelli M. Implant-supported prostheses esthetic
outcomes after socket preservation technique.
(2015) J Craniofac Surg 26:729-730. 2. Hae-Lyung Cho, Jae-Kwan Lee, Heung-Sik UM, Beom-Seok
Chang. Esthetic evaluation of maxillary single-tooth implants in the esthetic
zone. (2010) J Periodontal Implant Sci 40: 188–193. 3. Manjunath RG, Rana A, Sarkar A. Gingival Biotype
Assessment in a Healthy Periodontium: Transgingival Probing Method. (2015) J
Clin Diagn Res 9: ZC66-ZC69. 4. Frost NA, Mealey BL, Jones AA, Huynh-Ba G. Periodontal
Biotype: Gingival Thickness as it Relates to Probe Visibility and Buccal Plate
Thickness. (2015) J Periodontol 86:1141-1149. 5. Rasouli Ghahroudi AA, Khorsand A, Yaghobee S, Haghighati
F. Is biologic width of anterior and posterior teeth similar? (2014) Acta Med Iran 52: 697702. 6. Cochran DL, Obrecht M, Weber K, Dard M, Bosshardt D, et
al. Biologic width adjacent to loaded implants with machined and rough collars
in the dog. (2014) Int J Periodontics Restorative Dent 34: 773-779. 7. Reetika Gaddale, Jayashree Mudda, Ilangovan Karthikeyan,
Shrikar Desai, Harshada Hemchandra Shinde, et al. Determination of clinical
biologic width in chronic generalized periodontitis and healthy periodontium: A
clinicoradiographical study. (2015) J Indian Soc Periodontol 19: 194–198. 8. Yang Guang, Yan Minmin. Clinical observation and operation
designs of implant surgery in cases of maxillary central incisor lost with
insufficient alveolar bone. (2013) Stomatology 33: 245-247. 9. Traini T, Novaes AB, Piattelli A, Papalexiou V, Muglia
VA. The relationship between interimplant distances and vascularization of the
interimplant bone. (2010) Clin Oral Implants Res 21:822-829. 10. Gastaldo JF, Cury PR, Sendyk WR. Effect of the vertical
and horizontal distances between adjacent implants and between a tooth and an
implant on the incidence of interproximal papilla. (2004) J Periodontol
75:1242-1246. 11. Choquet V, Hermans M, Adriaenssens P, Daelemans P,
Tarnow DP, et al. Clinical and radiographic evaluation of the papilla level
adjacent to singletooth dental implants. A retrospective study in the maxillary
anterior region. (2001) J Periodontol 72: 1364-1371. 12. Lang NP, Loe H. The relationship between the width of
keratinized gingiva and gingival health. (1972) J Periodontol 43: 623-627. 13. Zhan Fuliang, Liu Ce, Liu Xianghua. The vital tooth
lesions lead to chronic maxillary sinusitis in 3 cases. (2013) China Practical
Journal of Department of Stomatology 6: 766-768. 15. Maillet M, Bowles WR, McClanahan SL, John MT, Ahmad M.
Cone-beam computed tomography evaluation of maxillary sinusitis. (2011) J Endod 37: 753-757. 16. Vaibhav Joshi, Shalini Gupta. Immediate Implant
Placement in Anterior Aesthetic Region and Assessment using Cone-Beam Computed
Tomography Scan Technology. (2015) J Int Oral Health 7: 99-102. Esthetic; Evaluation; Impact factor; Soft tissue
Principles of Soft Tissue Management in Dental Implants
Xiao-Quan Mao
Abstract
Full-Text
How Does One Evaluate Soft Tissue Esthetics?
The Impact Factors of Soft Tissue
Gingival biotype
Biologic width (BW)
The relationship between biotype and biologic width
Thickness of labial bone wall
Distance between implants
Distance between
Crown contact point and alveolar bone
Relationship between the distance of implants and CPB
Keratinized mucosa
width (KMW)
Condition of adjacent teeth
Suture
Discussion
List of Abbreviations
References
14. Cheng Yanan, Xu Pu, Jian Xinchun, Lu Liying, Zheng Tongwen, et al. Implant
failure for retrograde peri-implantitis.
(2013) Chinese Journal of Stomatology 48: 383-384. Keywords