Introduction
Congenital heart disease is a spectrum of structural problems of the heart or its major blood vessels which are present at birth due to failure of embryological development of fetus in the womb. VSD accounts for about 14-16% of all cases of congenital cardiovascular defects [1]. About eight of every 100 infants or 1% of live births is born every year with congenital cardiovascular defects. It is the number one cause of death from birth defect during the first year of life [1]. The defects can exist in isolation, can be complicated by additional intracardiac lesions, or can be part of more complex combinations, such as tetralogy of Fallot, double outlet right ventricle, transposition, or functionally univentricular hearts.
There are 4 subgroups defined in the guidelines, according to defect location: perimembranous, muscular, outlet and inlet type. The perimembranous type is the most frequent (about 80% of all VSDs) among adult population [2]. The clinical presentation and natural history can vary from small VSD with insignificant left-to-right shunt to VSD with significant left-to-right shunt with Left Ventricular (LV) volume overload and Right Ventricular (RV) pressure overload, which, if unrepaired, may cause pulmonary vascular disease and even Eisenmenger syndrome [3,4]. Patients with a small VSD and insignificant left-to-right shunt or with a repaired VSD usually remain event-free during follow-up.
However, several problems may still develop later in life, with the most important being endocarditis, LV dilatation due to volume overload, double-chambered right ventricle, Left Ventricular Outflow Tract Obstruction (LVOTO), Aortic Valve Regurgitation (AR) and complete heart block (especially in the earlier years of cardiac surgery) [2]. Though spontaneous closure in the first years of life is anticipated in cases of small defect; surgical repair is the gold standard treatment of VSD still yet. The main aim of this study is to observe the short term outcome of patch repair of VSD.
Materials and Methods
This study was conducted in Department of Pediatric Cardiac Surgery of Dhaka Shishu Hospital from May, 2017 to December, 2017. It is a prospective observational study. Initially all the patients admitted for VSD repair were enrolled by purposive sampling. The complicated cases where other congenital major deformities present were excluded from the study. A simple VSD which can be defined as an isolated VSD or a VSD with concomitant Atrial Septal Defect (ASP)/Patent Foramen Ovale (PFO), Patent Ductus Arteriosus (PDA) or mildly stenotic/regurgitant semilunar valves patients were included in this study.
At first, 56 patients were enrolled. Among them we kept only 50 patients according to the eligibility criteria. We prepared a pre-structured, peer-reviewed, interview and observation based data collection sheet. And we recorded pre, peri and postoperative data including sociodemographic, neonatal, on admission and perioperative clinical, biochemical and surgical variables. Surgical outcome and complications were assessed according to international criteria [5]. Primary objectives were to see immediate post-operative out-come, the number of ICU stay, Inotrope support and secondary objectives were to see any major post-operative complications. Safety parameters are also included, like the selection of the patient without any pre-operative infections, other major congenital malformations, lack surgeons experience and post-operative ICU care.
Data Analysis
All data were recorded, managed and analyzed with the help of Statistical Packages for Social Science (SPSS) version 23 (Ilinois, Chicago, USA). Frequencies and percentages were used for the qualitative variables median was used for data which were not normally distributed.
Results
Table 1 shows that the overall characteristics of patents where the mean birth weight and median weight at operation were 2.8 ± 0.73 kg and 5600 gram. Among 50 children, there were 22 (44%) boys and 28 (56%). On the contrary, 28 (56%) patients were in the group of ≤ 6 months and 22 (44%) patents were in the group of >6 months during operation. Table 2 shows that all 50 patients underwent patch repair due to volume load, repeated RTI and Failure to thrive in VSD. There were 2 types of VSD in this series. Out of 50 patent 46 (92%) had perimembranous type and 4 (8%) had double committed type.
The mean bypass and aortic cross clamp time was 70 ± 13.7 minutes and 35 ± 6.85 minutes respectively. The median postoperative mechanical ventilation duration and hospitalization duration were 0.4 (range: 0-26) days and 6 (3-43) days respectively.
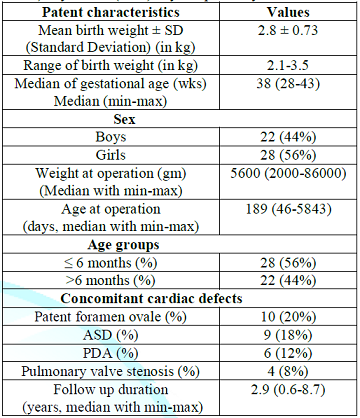
Table 1: Distribution of patients according to different characteristics (N=50).
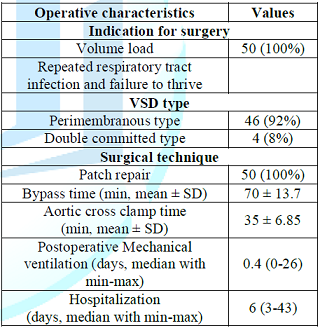
Table 2: Operative characterizes (N=50).
Table 3 shows that out of 50 patients with patch repair for VSD, 45 (90%) showed uneventful outcome whereas 2 (4%) patients suffered from post-operative pneumothorax. On the contrary, 1 (2%) patient each experienced chylothorax and transient heart block after surgery.
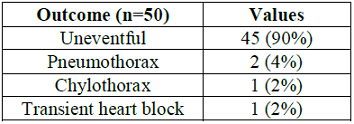

Table 3: Distribution of patients according to outcome (N=50).
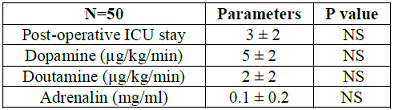
Table 4: Immediate Post-operative ICU parameters.
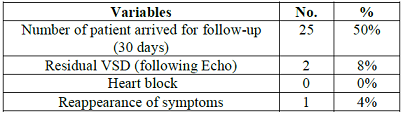
Table 5: Post-Operative Follow-up after discharge.
Surgical Technique
To perform intracardiac repair of VSD, median sternotomy was performed in all patients. All patients underwent cardiopulmonary bypass. Three surgeons from the different hospitals across the country performed the surgeries (Two surgeons performed 97.5% of the surgeries). We performed PTFE patch closure of all VSD, not a single direct closure was done. Concomitant closure of atrial septal defect closure, patent foramen ovale closure, patent ductus arteriosus ligation, infundibular muscle resection, valvuloplasty and/or division was done when needed. We selected the patients based on clinical symptoms and transthoracic Echocardiography, only one patient was checked for reversible pulmonary arterial hypertension by cardiac cath. After the operation on one Post-operative day, we performed a Transthoracic Echocardiogram to check the result. Before discharge another transthoracic Echocardiogram was performed in all cases (Figure 1 and 2).
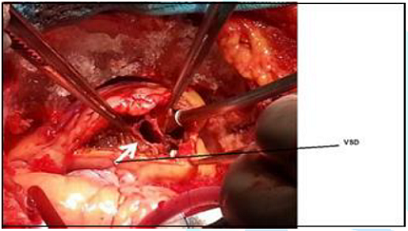
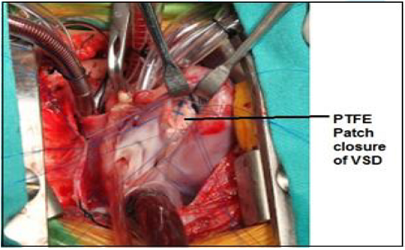
Figure 2: PTFE patch closure of VSD through right atriotomy.
Discussion
VSDs arise from failure of growth, alignment or fusion of one or more septal components and are best classified according to their margins and location [6]. A ventricular septal defect is a cardiac anomaly consisting of a connection between the right ventricle and the left ventricle. These defects can be single or multiple. A VSD may occur in any portion of the interventricular septum, including the membranous, muscular, inlet, or outlet septum, or a combination of locations. Perimembraneous VSD is the most common type of VSD (80%). Part of the defect is bordered by the fibrous continuity between the mitral and tricuspid valve. The defect may be partially or completely occluded by the septal leaflet of the tricuspid valve.
Muscular VSD is completely surrounded by muscular tissue. These defects are by definition located in the muscular part of the ventricular septum. Spontaneous closure of muscular VSDs frequently occurs in the first two years of life. Outlet VSD is formed by the continuity between the aortic and pulmonary valves. In this study, the mean birth weight of the respondents was 2.8 ± 0.73kg which was lower than the similar Dutch study where the mean birth weight was found, 3.14 (± 7.78) gm [7]. It was anticipated as the average growths of the neonates of Dutch countries are more standard than us due to average maternal nutritional deficit in our mothers in pregnancy.
On the contrary, the median weight at operation in our respondents was 5650 gm (range: 2000-86,000). The mean age at operation in the study of Saudi Arabia was higher than our reports [8]. The median age at operation in our aspect was 189 days (range: 46-5843 days). The similarities in the results were not observed in the previous study of Saudia Arabia where mean age at operation was higher [8]. It may be due to the poor performance status of our children. In our study, PFO (20%), ASD (18%), PDA (12%) and Pulmonary Valve Stenosis (PVS) (8%) were found as concomitant cardiac defect. These statistics were almost consistent with previous study.
Our all patients underwent patch repair where volume load, repeated respiratory tract infection and failure to thrive are the indications of surgery. There was no mortality observed in this study whereas major morbidity like pneumothorax (4%), chylothorax (2%) and transient heart block (1%) which was resolved within 7 days post operatively compare to Maartje, et al. study where it was 4.9% completed heart block was observed, which was 8% on that study, and other study showed it was 0.0-2.1% [9,10]. Outcome showed that 90% cases uneventful. However, ICU stay was 1-5 days, and some of them needed inotropic support in different doses. Mostly inotropes are used, dopamine, dobutamine and adrenaline, milrinone was not required. In the previous other studies the complications related to VSD repair were observed for less than the present report [11-13]. Three studies were conducted in the dedicated high volume centers where logistic supports are more modernized than our center.
Post-operative follow-up was the most challenging part, because patients were reluctant to visit due to low socioeconomic condition. Only 25 (50%) patients appeared on first 30 days follow-up. We havent included later follow-up periods in this study. Out of them post-operative Echocardiography shows 2 (8%) small residual VSD, expected to close spontaneously on later date, no complete heart block was observed. And 2 (4%) patients showed reappearance of symptoms, that is developed repeated respiratory tract infection, and congestive heart failure, for them dose of the drugs was adjusted accordingly.
Limitations of the Study
Being a developing country and poor socioeconomic status of the patient, the follow-up was quite challenging and also sample number was too little to come up a definitive conclusion.
Conclusion
In Bangladesh perspective where pediatric cardiac surgery is gradually gaining the popularity, there results can be claimed as excellent with no mortality and manageable morbidity.
References
1. Figueroa JDR, Magaña BDP, Hach JLP, Jiménez CC and Urbina CR. Heart malformation in children with Down syndrome (2003) Rev Esp cardiol 56: 894-899. https://doi.org/10.1016/S0300-8932(03)76978-4
2. Baumgartner H, Bonhoeffer P, De Groot NM, de Haan F, Deanfield JE, et al. ESC guidelines for the management of grownup congenital heart disease (2010) Eur Heart J 31: 2915-2957. https://doi.org/10.1093/eurheartj/ehq249
3. Penny DJ and Vick GW. Ventricular septal defect (2011) Lancet 377: 1103-1112. https://doi.org/10.1016/s0140-6736(10)61339-6
4. Soufflet V, de Bruaene VA, Troost E, Gewillig M, Moons P, et al. Behavior of unrepaired perimembranous ventricular septal defect in young adults (2010) Am J Cardiol 105: 404-407. https://doi.org/10.1016/j.amjcard.2009.09.047
5. Jacobs ML, OBrien SM and Jacobs JP. An empirically based tool for analyzing morbidity associated with operations for congenital heart disease (2013) J Thorac Cardiovasc Surg 145: 1046-1057. https://doi.org/10.1016/j.jtcvs.2012.06.029
6. Soto B, Becker AE, Moulaert AJ, Lie JT and Anderson RH. Classification of ventricular septal defects (1980) Br Heart J 43: 332-343. http://dx.doi.org/10.1136/hrt.43.3.332
7. Schipper M, Slieker MG, Schoof PH and Breur PM. Surgical Repair of Ventricular Septal Defect; Contemporary Results and Risk Factors for a Complicated Course (2017) Pediatr Cardiol 38: 264-270. https://doi.org/10.1007/s00246-016-1508-2
8. Ismail SR, Dughiem A, Abusuliman A, Kabbani M and Najm N. 803 Effect of Body Weight on the Outcome of Ventricular Septal Defect Repair (2012) Arch Dis Child 97: A230-A231. https://doi.org/10.1136/archdischild-2012-302724.0803
9. Maartje S, Martijn GS, Paul HS and Johannes MPJB. Surgical Repair of Ventricular Septal Defect; Contemporary Results and Risk Factors for a Complicated Course (2017) Pediatr Cardiol 38: 264-270. https://doi.org/10.1007/s00246-007-9016-z
10. Scully BB, Morales DL, Zafar F, McKenzie ED, Fraser CD, et al. Current expectations for surgical repair of isolated ventricular septal defects (2010) Ann Thorac Surg 89: 544-549. https://doi.org/10.1016/j.athoracsur.2009.10.057
11. Scully BB, Morales DL, Zafar F, McKenzie ED, Fraser CD Jr, et al. Current expectations for surgical repair of isolated ventricular septal defects (2010) Ann Thorac Surg 89: 544-549. https://doi.org/10.1016/j.athoracsur.2009.10.057
12. Anderson BR, Stevens KN and Nicolson SC. Contemporary outcomes of surgical ventricular septal defect closure (2013) J Thorac Cardiovasc Surg 145: 641-647. https://doi.org/10.1016/j.jtcvs.2012.11.032
13. Kogon B, Butler H, Kirshbom P, Kanter K and McConnell M. Closure of symptomatic ventricular septal defects: how early is too early? (2008) Pediatr Cardiol 29: 36-39. https://doi.org/10.1007/s00246-007-9016-z
*Corresponding author:
Kazi Zahidul Hoque, Assistant Professor (Consultant) and Unit Chief, Pediatric Cardiac Surgery Unit 2, Dhaka Shishu (Children) Hospital and Institute of Child Health, Consultant, Metropolitan Medical Center, Dhaka 1207, Bangladesh, Tel: +8801711352549, E-mail: kzhoque72@yahoo.com
Citation:
Hoque ZK, Chowdhury GM, Islam A, Hossain M, Rahman M, et al. Surgical repair of VSD and their short term outcome in a tertiary care hospital (2019) Clinical Cardiol Cardiovascular Med 3: 34-37.
Keywords
Ventricular Septal Defect, Pediatric Cardiology, Cardiac complications.


 PDF
PDF