Introduction
The topographical orientation system, also known as the spatial navigation, topo-kinetic and action-extrapersonal systems, is one of the four major networks in the brain governing our interaction with our 3D environment [1]. It is believed to be composed mainly of subcortical regions such as the caudate nucleus and anterior thalamus and three posterior regions-the medial-temporal lobe/hippocampus, posterior cingulate, and parietal-temporal cortex [1-3]. It is the system responsible for scene and route memory, a sense of presence in the world, and topographical orientation and way finding in the plane of the Earths surface [1].
It is widely accepted that the topographical memory component of this system is centered in the hippocampus. Activation of the hippocampus occurs during recall of topographical routes [4] whereas damage to it results in amnesia for spatial landmarks and maps and severe topographical disorientation [5]. Although the topographical memory system deteriorates during normal aging [6-8], severe disruption of it is a very early diagnostic sign of Alzheimers disease [8-15]. Indeed, atrophy and/or metabolic deactivation of key components of the topographical neural network are among the best predictors of impending Alzheimers disease [16-19].
Despite their neurophysiological basis and good predictive validity, topographical tests are not routinely used in assessment of early Alzheimers disease.
The purpose of the present study, therefore, was to compare topographical versus more widely used non-topographical measures of cognitive ability in older adults. To test topographical memory, three tests were used in the present study:
1. The Camden Topographical Recognition Memory Test (CTRMT)
2. A computerized Topographical Mental Rotation Test (TMRT) similar to the “four mountains” test used by Bird et al. [9] and Hartley and Harlow [20].
3. A VirtualPond Maze (VPM) similar to the widely used Morris water maze in rodents and virtual mazes that have been developed for humans [21-23]. While the CTRMT has not been specifically linked to hippocampal function, memory for distinct scenes is dependent on this region [24,25]. Memory for scenes requiring topographical mental rotation is also dependent on the hippocampus and the critical role of the hippocampus in the water maze has been repeatedly shown in both animals and humans [20-22].
The tests of non-topographical function were the Montreal Cognitive Assessment (MoCA), the Trail-Making Test Part B (TMT-B), and a computerized Visual Short-Term Memory Task (VSMT) that had a similar appearance to the TMRT except that it involved a matching-to-sample object recognition memory rather than a topographical transformation. Even though it was a basis for screening of the participant population, the MoCA ended up replacing a different non-topographical test-the Camden Short Recognition Memory Test for Words-because scores on the latter severely violated normality due to a ceiling effect.
To determine relationships within and across the two sets of measures, a biserial correlation matrix and factor analysis were performed on scores from the six measures.
Methods
Participants
A total of 25 active individuals between the ages of 70 and 85 participated in this study. All participants were prescreened for dementia and those scoring less than 19 on the MoCA-the recommended cutoff for the normal designation for a similar age sample-were excluded from the study [26]. All but two of 27 originally recruited participants that met other exclusionary criteria achieved the MoCA criterion. Participants were additionally excluded if they had ever suffered a stroke, seizure, traumatic brain injury, or had a diagnosed neurologicalcondition. Finally, participants were excluded if they were currently taking any psychoactive drugs and engaged in other than moderate caffeine consumption (no more than 300 mg per day, the equivalent of three cups of coffee per day), moderate alcohol consumption, and mild pain medication (used by two participants). Participants signed an informed consent document approved by Biomed IRB (Biomedical Institute of America; San Diego, CA).
Apparatus
All cognitive testing was performed in an outpatient office setting and required approximately 90 min. Two of the three topographical tests (the VPM and TMRT) were programmed for this study and administered using a Compaq NC6400 computer (Hewlett-Packard) under moderately dim illumination in a quiet room while the participant was seated. The third topographical test was the CTRMT, administered from a test booklet using standardized procedures in a well-lit room [27].
The three non-topographical tests were the MoCA (which includes a clock-drawing
and a Necker-Cube copying task but no topographical assessment per se), the
TMT-B, and a computerized short-term visual memory test. The MoCA and the TMT-B
were administered as paper-and-pencil tests, while the VSMT was programmed for
this study and also administered on the Compaq NC6400 computer. These tests
were carried out as part of a larger study that also analyzed several measures
of vestibular function and their relationship to topographical abilities with
vestibular testing performed in a separate facility [28].
Tests
Camden Topographical Recognition Memory Test (CTRMT):
This task required participants to view 30 urban scenes during a 3-s interval and report whether the photograph was taken by an amateur or a professional photographer. Immediately after the completion of the presentation sequence, participants were shown the same 30 scenes in a different order along with two never-before-seen versions of each scene taken from different distances and egocentric viewing perspectives. In a three-alternative forced-choice recognition procedure with self-pacing, participants were then required to point to the scene that was originally presented. Each score was based on the total correct out of 30.
Virtual Pond Maze (VPM): Participants
started from one of six locations around the virtual pond, surrounded by six
houses and six trees, all evenly spaced such that each starting location
provided a unique set of spatial landmarks (see Figure 1, right panel). Using only the left and right cursor
arrows, participants were required to navigate to a fixed platform slightly
offset from the middle of the pond, with the forward speed set by the computer
at a simulated 7 m/s. The location and size of the platform was set such that
participants had to make at least one cursor correction to reach the platform
from each of the starting points. A cutoff value of 60 s was imposed to end the
trial, which many participants reached, especially from the more remote
starting points.
After approximately 20 min of instructions and practice, participants were
tested on 18 trials, consisting of one platform-visible trial followed by two
platform-nonvisible trials, in which spatial memory was required to reach the
platform. The performance measures were the time taken to reach the platform,
the virtual distance travelled, and the number of corrections made. Only the
time to reach the platform was included in the final analysis, since the number
of corrections partly involved strategy and the virtual distance almost
perfectly correlated with, and was therefore redundant to, the time to reach
the platform. Also, participants reached the platform rapidly and with little
variation in the visible trials (a “ceiling effect”), presumably because
forward speed was set by the computer; thus, only data from the nonvisible
trials were used to assess navigational memory.
Topographical Mental Rotation Test (TMRT): Participants viewed a scene containing a set of three objects (e.g., red cylinder, blue sphere, green cube) and were then shown a figure instructing them to rotate their viewpoint 90º left, 90º right, or 180º opposite (see Figure 1, left panel). They were then shown three scenes from each of the rotated viewpoints and asked to click on the image that depicted the correct viewpoint shift. A yellow box indicated the participants choice while a green box (appearing only during practice trials) showed the correct viewpoint. Participants had 12 s to view each scene and 14 s to make their response, with a timer appearing during the last 5 s of the forced-choice interval. After being presented with instructions, which included demonstrations of the task using actual objects, participants viewed a set of 12 practice trials (they could view a second set if they chose to) and then were presented with 15 test trials. Each score was based on the total number of correct responses out of 15.
Montreal Cognitive Assessment (MoCA): The MoCA consists of 30 points derived from a set of 12 tasks, including a miniature version of the trail-making task (1 pt), a Necker cube copy (1 pt), clock drawing (3 pts), naming (3 pts), delayed recall (5 pts), forward and reverse digit span (2 pts), go/no-go attention (1 pt), serial-seven subtraction (3 pts), sentence repetition (2), verbal fluency (1 pt), verbal analogous reasoning (2 pts), and general orientation (6 pts) (see www.mocatest.org ) Testing on the MoCA required about 10 min [29]
Trail-Making Test Part B (TMT-B): The TMT consists of two tasks: Part A, which presents a connect-the-dots sequencing and visual scanning task for numbers only; and Part B, which requires alternate sequencing of numbers and letters. Each task is preceded by a sample that provides for training and practice. The dependent variable was time to completion, with timing beginning immediately after the participant began to move the pencil. Errors were corrected immediately by returning the participant to the last correct point in the sequence, in accordance with standardized administration procedures. Only time to completion for Part B was included in the final analysis.
Visual Short-Term Memory Test (VSMT): This task was designed as a non-topographical comparison to the TMRT. The stimuli and grid were identical to the TMRT task shown in Figure 1, except that four objects were presented rather than three. However, the task differed in that the viewing perspective and spatial locations of the objects never changed during the testing phase; rather, the three test stimuli consisted of the original scene and two scenes in which one of the four objects in the original scene changed its shape or color (but not both). In the two discrepant scenes, the same object could change in different ways (e.g., a red sphere could become a red cube in one scene or a blue sphere in the other) or different objects could change in the same (both color changes) or different ways (e.g., a blue sphere could change to a green sphere in one scene while a yellow cone could turn into a yellow cube in the other). Participants had 9 s to view each scene and 12 s to make their response, with a timer appearing during the last five seconds of the forced-choice interval. As in the TMRT, participants were required to click on the original image during the recognition period, which caused a yellow box to appear over their selection while a green box surrounded the correct response (green box appeared only during practice trials). After being presented with instructions, participants viewed a set of 12 practice trials (they could view a second set if they chose to) and then were presented with 15 test trials. Each score was based on the total number of correct responses out of 15.
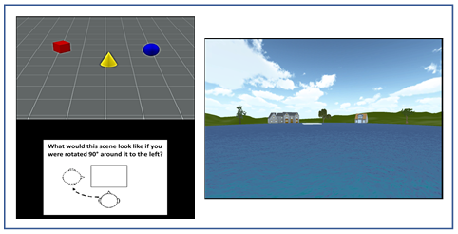
Figure 1: An illustration of the stimuli used in the TMRT task (left) and pond maze (right).
Analysis
A total of six variables were analyzed in this study: CTRMT (# correct), TMRT (# correct), VPM (time to completion), MoCA (# correct), TMT-B (time to completion), and VSTMT (# correct). SPSS (IBM, Chicago, IL) was used to perform an exploratory factor analysis on the data using a varimax rotation and Kaiser Normalization. Because higher scores (times) on the VPM and TMT-B reflected poorer performance whereas higher scores on the other four tests reflected better performance, time to completion scores on the VPM were subtracted from the cutoff time of 60 s whereas times on the TMT-B were subtracted from the maximum time in the study (164 s). Longer times on the VPM and TMT-B now reflected better performance, without otherwise transforming the data; hence, the correlation between the actual and inverted times was -1.0 for both measures.
A “composite” topographic measure was created by turning the three
raw topographic scores for each participant into percentiles, based on established norms (in the case of the CTRMT) or the present studys means and standard deviations (for the VPM and TMRT scores), and then averaging all three together.
Results
The sample consisted of 16 females and nine males, with an average age of 76.4 years. Nine of the 25 participants were Hispanic, 12 were non-Hispanic Caucasians, three were Asian-Americans, and one self-described as “other”. In terms of education level, seven had high-school degrees, six had college degrees, and 12 had graduate degrees.
The means and standard deviations for the six cognitive measures are shown in (Table 1). The complete correlation matrix containing all 21 bivariate correlations is shown in (Table 2), while the results of the exploratory factor analysis are shown in (Table 3).
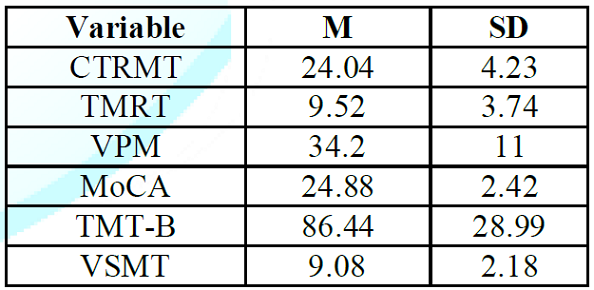
Table 1: Means and Standard Deviations for the Topographical and Non-topographical Measures.
On the tests in which number of correct was measured, mean performance ranged from slightly over 60% (TMRT and VSMT) to slightly over 80% (MoCA and CTMRT). The average score on the CTRMT, MoCA and TMT-B tests were similar to age-adjusted norms from previous studies [26, 30-31].
Many participants had trouble with the VPM, TMRT, and VSMT, either exceeding the cutoff time in the case of the VPM or scoring at chance levels or below on the TMRT and VSMT. The largest variability (as a percentage of the mean) occurred in the TMRT test, partly because of a large (>50%) gender difference, with males averaging 12.44 correct and females averaging 7.8 correct. No other measure yielded a gender difference of more than 15%.
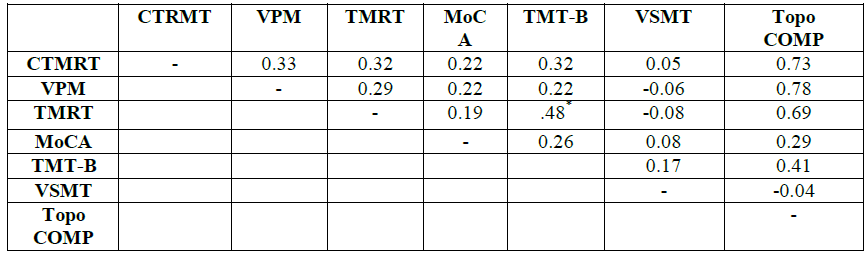
The bivariate correlation matrix is shown in Table 2. Because scores on all but one of the six measures violated normality according to the Shapiro-Wilk statistic, Spearmans rho was used to determine all correlations.
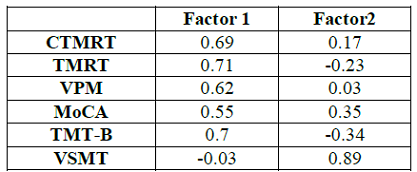
Table 3: Factor Loadings on Principal Components.
Only one correlation-that between the TMRT and TMT-B scores-proved significant, with the correlations among the three topographical measures ranging from 0.29 to 0.33. The correlations between each of the three topographic measures and the topographical composite score ranged from 0.69 to 0.78; these high correlations would be expected in that each of the topographic scores contributed a third to the composite score. The correlations between the topographical composite and the non-topographic scores were much more modest, the highest (0.41) being the TMT-B-composite one.
The results of the factor analysis revealed two principal components with eigenvalues greater than 1.0 that accounted for 54.6% of the variance (Factor 1=36.1%; Factor 2=18.5%). The loadings for each of the six variables on each factor are shown in Table 3. The three topographical variables loaded very highly on Factor 1 (0.69, 0.62. and 0.71, for the CTMRT, VPM, and TMRT measures, respectively) but loaded poorly on Factor 2 (0.17, 0.03, and -0.23, for those same variables). Hence, it may be concluded that Factor 1 is related to topographical abilities. The TMT-B also loaded highly on Factor 1 (0.70) and the MoCA moderately no (“0.55), while the VSMT loaded poorly (-0.03). Conversely, the three non-topographic measures loaded better than the topographic ones on Factor 2.
To illustrate further the dissociation between the topographical and non-topographical measures, MoCA scores for the four participants with the highest topographical composites (range=23-27, M=25.5) overlapped the MoCA scores for the four participants with the lowest topographical composites (range=19-27, M=23.25). In fact, the participants with the two lowest topographical composites (6th and 16th percentile) scored near- and above-average on the MoCA (23 and 27, respectively, relative to the sample mean of 24.88).
Discussion
The results of this preliminary study show dissociation between topographical and non-topographical measures of cognitive function. Despite some limitations of this study that will be addressed, this result could hold potentially important implications for future screening for mild cognitive impairment and early Alzheimers dementia.
The two principal components derived from the factor analysis distinguished the topographical measures from the non-topographical measures. The topographical memory measures all loaded highly on the first factor (>.6) but poorly on the “non-topographical” factor (<.25). The reverse was true for the visual memory test, which loaded highly on the second factor (.89) but poorly on the “topographical” factor (-.03). The TMT-B also loaded very well on the “topographical” factor (.70) and the MoCA somewhat (.55), but they also loaded more strongly than the topographical measures on the second factor, which presumably involved non-topographical memory ability. The results of the factor analysis must be viewed with caution, however, given that the sample size was relatively small and none of the bivariate correlations between the topographical measures proved statistically significant.
It is unclear why the bivariate correlations among the topographical memory measures were so modest, given their loadings on the “topographical” factor. Although the three topographical memory measures have been shown to tap into hippocampal function [9, 20-22, 24-25], it is likely that they represent slightly different cognitive processes. It has previously been shown that topographical memory and active navigation are not always well correlated [10]. Moreover, the gender bias only in the TMRT suggests that it additionally reflects some of the same spatial rotational processes previously shown to be superior in males [32], possibly involving the parietal-temporal portion of the topographical memory system. It may very well be the case that poor performance on a single topographical test is of less clinical significance than a global topographical impairment, as assessed by a composite topographical score.
The partial dissociation between the topographical and non-topographical measures in this study has potentially important implications for screening for Alzheimers disease. Although widely used measures of dementia such as the MoCA and TMT-B may tap into topographical abilities and even hippocampal function in the latter case, they are also dependent on other brain areas such as the frontal lobes, which fail later in the time-course of Alzheimers disease. [33,34]. The TMT-B requires cognitive shifting and other executive functions, while the MoCA is mostly composed of verbal and working-memory items. While the TMT-B can discriminate the mildly cognitively impaired from healthy controls [11,35], it may not be as sensitive as pure topographical measures in diagnosing the initial topographical deficit in Alzheimers [11,15].
Of the topographical tests, the CTRMT may be the most advantageous in that it
is standardized, normed, easy to administer, and achievable by all
participants, in addition to loading highly on composite “topographical” factor
measures.
More studies with larger sample sizes are required to determine if current
widely used cognitive measures are as effective as specific topographical ones
in the earliest prediction of Alzheimers.
Acknowledgements
We wish to acknowledge the assistance of Sam Washburn (computer programming), Dr. Michael Roman (neuropsychological testing), Dr. Dora Angelaki (experimental protocol), John Hatch (statistics) and Karl McCloskey (administrative).
Research reported in this publication was supported by the National Center for Advancing Translational Research (NCATS); the National Institute on Aging (NIA); and the National Heart, Lung and Blood Institute (NHLBI) under Award #TR000645-01. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health.
References
1. Previc FH. The neuropsychology of 3-D space (1998) Psychol Bull 124: 123-64. https://psycnet.apa.org/doi/10.1037/0033-2909.124.2.123
2. Berthoz A. Parietal and hippocampal contribution to topokinetic and topographic memory (1997) Philos T Roy Soc B 352: 1437-1448. https://doi.org/10.1098/rstb.1997.0130
3. Maguire EA, Burgess N, Donnett JG, Frackowiak RS, Frith CD, et al. Knowing where and getting there: A human navigation network (1998) Science 280: 921-924. https://doi.org/10.1126/science.280.5365.921
4. Maguire EA, Frackowiak RS and Frith CD. Recalling routes around London: activation of the right hippocampus in taxi drivers (1997) J Neurosci 17: 7103-7110. https://doi.org/10.1523/jneurosci.17-18-07103.1997
5. Aguirre GK and DEsposito M. Topographical disorientation: A synthesis and taxonomy (1999) Brain 122: 1613-1628. https://doi.org/10.1093/brain/122.9.1613
6. Adamo DE, Briceno EM, Sindone JA, Alexander NB and Moffat SD. Age differences in virtual environment and real world path integration (2012) Front Aging Neurosci 4: 26. https://doi.org/10.3389/fnagi.2012.00026
7. Moffat SD, Elkins W and Resnick SM. Age differences in the neural systems supporting human allocentric spatial navigation (2006) Neurobiol Aging 27: 965-972. https://doi.org/10.1016/j.neurobiolaging.2005.05.011
8. Monacelli AM, Cushman, LA, Kavcic V and Duffy CJ. Spatial disorientation in Alzheimers disease: The remembrance of things passed (2003) Neurology 61: 1491-1497. https://doi.org/10.1212/wnl.61.11.1491
9. Bird CM, Chan D, Hartley T, Pijnenburg YA, Rossor MN, et al. Topographical short-term memory differentiates Alzheimers disease from frontotemporal lobar degeneration (2010) Hippocampus 20: 1154-1169. https://doi.org/10.1002/hipo.20715
10. Boccia M, Di Vita, A, Diana, S, Margiotta, R, Imbriano L, et al. Is losing ones way a sign of cognitive decay? Topographical memory deficit as an early marker of pathological aging (2019) J Alzheimers Dis 68: 679-693. https://doi.org/10.3233/jad-180890
11. Chan D, Gallaher LM, Moodley K, Minati L, Burgess N, et al. The 4 Mountains test: A short test of spatial memory with high sensitivity for the diagnosis of pre-dementia Alzheimers disease (2017) J Visual Exp 116: 54454. https://doi.org/10.3791/54454
12. Guariglia CC and Nitrini R. Topographical disorientation in Alzheimers disease (2009) Arq Neuropsiquiatr 67: 967-972. https://doi.org/10.1590/s0004-282x2009000600001
13. Pengas G, Patterson K, Arnold RJ, Bird CM, Burgess N, et al. Lost and found: Bespoke memory testing for Alzheimers disease and semantic dementia (2010) J Alzheimers Dis 21: 1347-1365. https://doi.org/10.3233/jad-2010-100654
14. Previc FH. Vestibular loss as a contributor to Alzheimers disease (2013) Med Hypotheses 80: 360-367. https://doi.org/10.1016/j.mehy.2012.12.023
15. Wei EX, Oh ES, Harun A, Ehrenburg M and Agrawal Y. Vestibular loss predicts poorer spatial cognition in patients with Alzheimers disease (2018) J Alzheimer Dis 61: 995-1003. https://doi.org/10.3233/jad-170751
16. Huang C, Wahlund LO, Svensson L, Winblad B and Julin P. Cingulate cortex hypoperfusion predicts Alzheimers disease in mild cognitive impairment (2002) BMC Neurol 2: 9. https://doi.org/10.1186/1471-2377-2-9
17. Johnson NA, Jahng GH, Weiner MW, Miller BL, Chui HC, et al. Pattern of cerebral hypoperfusion in Alzheimer disease and mild cognitive impairment measured with arterial spin-labeling MR imaging: Initial experience (2005) Radiology 234: 851-859. https://doi.org/10.1148/radiol.2343040197
18. Lithfous S, Dufour A and Després O. Spatial navigation in normal aging and the prodromal stage of Alzheimers disease: Insights from imaging and behavioral studies (2013) Ageing Res Rev 12: 201-213. https://doi.org/10.1016/j.arr.2012.04.007
19. Mosconi L. Brain glucose metabolism in the early and specific diagnosis of Alzheimers disease. FDG-PET studies in MCI and AD. (2005) Eur J Nucl Med Mol I 32: 486-510. https://doi.org/10.1007/s00259-005-1762-7
20. Hartley T and Harlow R. An association between human hippocampal volume and topographical memory in healthy young adults (2012) Front Human Neurosci 6: 338. https://doi.org/10.3389/fnhum.2012.00338
21. Sharma S, Rakoczy S and Brown-Borg H. Assessment of spatial memory in mice. Life Sci (2010) 87: 521-536. https://doi.org/10.1016/j.lfs.2010.09.004
22. Brandt T, Schautzer F, Hamilton DA, Bruning R, Markowitsch HJ, et al. Vestibular loss causes hippocampal atrophy and impaired spatial memory in humans (2005) Brain 128: 2732-2741. https://doi.org/10.1093/brain/awh617
23. Moffat SD and Resnick SM. Effects of age on virtual environment place navigation and allocentric cognitive mapping (2002) Behav Neurosci 116: 851-859. https://doi.org/10.1037//0735-7044.116.5.851 24. Epstein R and Kanwisher N. A cortical representation of the local visual environment (1998) Nature 392: 598-601. https://doi.org/10.1038/33402
24. Epstein R and Kanwisher N. A cortical representation of the local visual environment (1998) Nature 392: 598-601.
25. Bonnici HM, Kumaran D, Chadwick MJ, Weiskopf N, Hassabis D, et al. Decoding representations of scenes in the medial temporal lobes (2012) Hippocampus 22: 1143-1153. https://doi.org/10.1002/hipo.20960
26. Trzepacz PT, Hochstetler H, Wang S, Walker B, Saykin AJ, et al. Relationship between the Montreal Cognitive Assessment and Mini-mental State Examination for assessment of mild cognitive impairment in older adults (2015) BMC Geriatr 15: 107. https://doi.org/10.1186/s12877-015-0103-3
27. Warrington E. The Camden memory tests manual (1996) East Sussex, England: Psychology Press, UK
28. Previc FH, Krueger WW, Ross RA, Roman MA and Siegel G. The relationship between vestibular function and topographical memory in older adults (2014) Front Integr Neurosci 8: 1-8. https://doi.org/10.3389/fnint.2014.00046
29. Nasreddine ZS, Phillips NA, Bedirian V, Charbonneau S, Whitehead V, et al. The Montreal Cognitive Assessment, MoCA: A brief screening tool for mild cognitive impairment (2005) J Am Geriatr Soc 53: 695-699. https://doi.org/10.1111/j.1532-5415.2005.53221.x
30. Lee DM, Tajar A, Ulubaev A, Pendleton N, ONeill TW, et al. The association between different cognitive domains and age in a multicentre study of middle-aged and older European men (2009) Int J Geriatr Psych 24: 1257-1266. https://doi.org/10.1002/gps.2255
31. Tombaugh TN. Trail Making Test A and B: Normative data stratified by age and education (2004) Arch Clin Neurol 19: 203-214. https://doi.org/10.1016/s0887-6177(03)00039-8
32. Nazareth A, Herrera A and Pruden SM. Explaining sex differences in mental rotation: Role of spatial activity experience (2013) Cogn Process 14: 201-204. https://doi.org/10.1007/s10339-013-0542-8
33. Leirer VM, Wienbruch C, Paul-Jordanov I, Kolassa S, Elbert T, et al. Hippocampal activity during the transverse patterning task declines with cognitive competence but not with age (2010) BMC Neurosci 11: 113. https://doi.org/10.1186/1471-2202-11-113
34. Stuss DT, Bisschop SM, Alexander MP, Levine B, Katz D, et al. The Trail-Making Test: A study in focal lesion patients (2001) Psychol Assessment 13: 230-239. https://doi.org/10.1037//1040-3590.13.2.230
35. Ashendorf L, Jefferson AL, OConnor MK, Chaisson C, Green RC, et al. Trail making test errors in normal aging, mild cognitive impairment, and dementia (2008) Arch Clin Neuropsych 23: 129-137. https://doi.org/10.1016/j.acn.2007.11.005
Corresponding author
Previc FH, Biomedical Development Corporation, 620 East Dewey Place, San Antonio 78212, Texas, USA, Tel: +612434014044, E-mail: fprevic@sbcglobal.net
Citation
Previc FH, Ross RA and Siegel G. Dissociation of measures of topographical and non-topographical cognitive ability in older adults (2019) Neurophysio and Rehab 2: 47-51
Keywords
Topographical, Memory, Hippocampus, Elderly, Alzheimers.


 PDF
PDF