Introduction
The global burden of essential hypertension and associated co-morbidities (cardiac failure, renal failure) is rising continuously [1]. Despite the availability of newer drugs for hypertension, the epidemic is not under control especially in developing countries [2,3]. Hypertension is a state of vascular system where the whole body vasculature is set at a particular level for a particular person [4]. BP>140/90 according to JNC7 is hypertension [5]. Lifestyle modification and the use of 2-4 antihypertensive agents are recommended at various stages of hypertension (JNC8) [6]. Despite triple-drug therapy, blood pressure control is only mild to moderate especially in the elderly [7]. This review emphasizes primarily the physiologic aspect of blood pressure control; possible role of VMC and its connections with the hypothalamus and cortex (indirectly) in the development of high blood pressure and secondarily role of adding stress-relieving (stress and mental exhaustion) methods in lifestyle measures to prevent an epidemic of hypertension [8-10].
Review of Literature
Textbook of physiology and various reference studies have been reviewed [8-35]. We will discuss the review in the following sections.
Physiology of Blood Pressure Control-Role of Vasomotor Center
The vasomotor center is located bilaterally in the reticular substance of the medulla and lower third of pons. This center has a vasoconstrictor area that sends sympathetic impulses to reach via the spinal cord to arterioles, arteries and virtually all organs. A vasodilator area sends an impulse via vagus nerve is less predominant and a sensory area, nucleus of tractus solitaries which receives signals from baroreceptors and send it to vasoconstrictor or vasodilator area. Under normal conditions, the vasoconstrictor area transmits signals continuously to the sympathetic nerve fibers releasing a small amount of noradrenaline at nerve endings maintaining basal sympathetic tone. This vasomotor center sets blood pressure at a particular level. This message is conveyed to each vessel and heart via sympathetic discharge. The vasomotor center is influenced by many parts of the cerebral cortex has an excitatory or inhibitory effect on the vasomotor center. Stimulation of anterior temporal lobe, the orbital areas of the frontal cortex, and the anterior part of the cingulate gyrus, the amygdala, the septum, and the hippocampus can excite or inhibit the vasomotor center. The hypothalamus exerts a powerful excitatory or inhibitory effect on the vasomotor center.
Thus it plays an important role in controlling the vasoconstrictor system. The basal sympathetic tone decides the cardiac contractility, arteriolar resistance in resting state. For example, at blood pressure 120/80 mm Hg the VMC is set at 120/80 whole body vasculature and cardiac contractility is maintained at that level to produce B.P. at this level. The RAAS (RAAS-Renin Angiotensin Aldosterone System) also is set accordingly. VMC has a dual relationship in maintaining blood pressure, on one hand, it has self-tone influenced by the hypothalamus and various cortical areas, on the other hand, it is connected to baroreceptors and adjusts blood pressure according to their signals (Flow chart 1) [4,8].

Flow chart 1: Normal physiology-Normal Blood Pressure.
Pathophysiology
of High Blood Pressure
The pathophysiology of hypertension is still not clear. Various
mechanisms including sympathetic nervous system over activity genetics, excess
salt intake and pressure natriuresis, obesity, OSA (Obstructive Sleep Apnea), insulin resistance, nitric
oxide pathway, and hypertension and its association with increased basal
sympathetic discharge-cortical connections have been mentioned [9,11-19]. The
maximum association of essential hypertension is found with sympathetic over
activity directly or indirectly involved in different mechanisms of
hypertension including OSA, insulin resistance, obesity, endothelial dysfunction
RAAS etc. [20-23]. It is the increased basal sympathetic discharge and not
overt discharge. Overt discharge is mainly present in white coat hypertension.
At the beginning (normotensive state), there is an elevation in basal sympathetic discharge which increases LV Ejection Force (LVEFO) shifts blood pressure from normotensive to stage 1 and then to stage 2 and further shifts from one value to further higher values into stage 2 [24]. There is a resetting of the whole body system including cardiac output according to that new blood pressure level. Though sympathetic discharge may come down to normal after shifting, now the whole-body system, all receptors are set to a newer level so even if sympathetic activity comes back to normal, B.P. does not return to normal. There is a certain adaptation of the baroreceptor and renal mechanism to a newer level.
Reasons for
Elevated Basal Sympathetic Discharge
It is clear from previous studies that this discharge is central in
origin. How basal rhythm is disturbed? Possibly persistent-stress, mental
overwork, fast mental speed disturbs cortical influences (desynchronization; associated with low voltage
fast Beta activity in Electroencephalography-EEG) to hypothalamus and shifts
VMC to a higher level (possible resetting of VMC) and therefore basal discharge
increases. So there are two situations one if blood pressure is high VMC tries
to bring back to normal (normal physiology) two is that if VMC is set at a
higher level it will give more basal sympathetic discharge and bring the blood
pressure or whole body vasculature to the same higher level of VMC (Flow chart 2) [8,9,24].
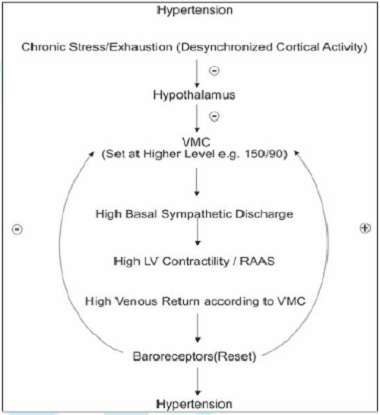
Flow chart 2: Hypertension? Shift of VMC.
Consequences
of Resetting of VMC at Different Levels
Once VMC is set at a particular level blood pressure is set at that
level, to achieve blood pressure at that level cardiac contractility, stroke
volume, venous return, Renin-Angiotensin level, vascular tone, etc. are set
accordingly. For example, systolic blood pressure 120 mmHg has lesser values
for all these parameters as compared to 140 mmHg systolic blood pressure and
further less if blood pressure is 160 mmHg. One may find high LV (Left Ventricular) contractility (ejection force)/LVEFO,
high renin levels at a high blood pressure level. So the whole body system
operates according to the VMC level.
Conclusion
(Pathophysiology)
For the development of hypertension, there is a possible resetting of
VMC at a higher level. Starting from cortical impulses to the hypothalamus
there is a shift of VMC at a higher level followed by high basal sympathetic discharge and increased LV ejection force
there is shifting of baroreceptors and renal mechanism to a new higher level
along with BP. Repetition of the same process shifts BP even higher.
Available
Antihypertensive Treatment
(Joint National Committee)
JNC 7: According
to JNC 7 guidelines for Hypertension, two or more antihypertensive drugs will be required to control
hypertension to goal in most patients i.e. to under 140/90 mm of Hg, or less
than 130/80 mm of Hg for patients with diabetes or chronic kidney disease. It
was suggested that a blood pressure goal of less than 140/90 mm Hg, lifestyle
modification, and polytherapy, e.g. a thiazide diuretic for stage 1
hypertension (<160/100 mmHg) and combination therapy with a thiazide
diuretic and an Angiotensin-Converting Enzyme (ACE) inhibitor, Angiotensin II
Receptor Blocker (ARB), or calcium channel blocker for stage 2 hypertension (≥
160/100 mmHg) [5].
JNC 8-Lifestyle Changes: According to JNC 8-various lifestyle changes have been suggested including cessation of smoking, control of blood glucose and lipids, healthy diet, moderate alcohol consumption, reduced sodium intake, that is, less than 2400 mg per day and, moderate to vigorous physical activity 3-4 times a week. Drug Therapy in JNC 8-First-line drugs for Hypertension is Thiazide diuretics, ACE inhibitors, ARBs and Calcium Channel Blockers (CCBs). Beta-blockers are no longer considered as first-line drugs. ACE inhibitors/ARBs are the first choice drugs in patients with Chronic Kidney Disease (CKD) irrespective of ethnic backgrounds. For African descent patients without CKD, calcium channel blockers or thiazides are preferred. The goal for all patients<60 years, BP should be<140/90 mmHg, irrespective of presence or absence of diabetes DM (Diabetes Mellitus) or CKD. The goal for the elderly>60 years without CKD or DM or both, BP is targeted at<150/90 mm/Hg. The goal for elderly>60 years with CKD or DM or both, BP is targeted at<140/90 mmHg.
ACC 2017 Guidelines/Recommendations for Hypertension Management: According to American College of Cardiology (ACC) 2017 patients are categorized into normal (<120 mmHg SBP), elevated (120-129 mmHg SBP), stage-1 (130-139 mmHg SBP) and stage-2 (>140 mmHg SBP) hypertension. Detection of white coat hypertension and masked hypertension is required. Regular follow-up is also mandatory. Non pharmacologic intervention includes weight loss (at least 1 kg for overweight), Healthy diet (rich in fruits/vegetables/whole grains), reduced intake of dietary sodium (1000 mg reduction in a day) increase potassium intake, enhance physical activity (aerobic/dynamic resistance/isometric resistance) 3 sessions per week, moderate alcohol intake (men<2 drinks daily/women<1 drink daily). Oral antihypertensive therapy categorizes into three
· Primary agents-Thiazide type diuretics (Chlorthalidone, Hydrochlorthiazide)/ACE inhibitors (Ramipril, Lisinopril)/ARBs (Azilsartan, Candesartan)/CCB-dihydropyridine (Amlodipine, Nifedipine)/CCB-nondihydropyridine (Diltiazem).
· Secondary agents-loop diuretics (Torsemide), Potassium-sparing diuretics, Beta-blockers (cardioselective-atenolol, along with vasodilatory property Nebivolol), Renin inhibitors and alpha-1 blockers. Centrally Alpha2-agonists (Clonidine, Moxonidine) and other centrally acting drugs are reserve drugs as the last line due to side effects.
· CVD (Cardiovascular Disease) risk and hypertension goal-A) Clinical CVD or 10 year (Atherosclerotic Cardiovascular Disease) ASCVD risk>10% (BP goal<130/80), B) No clinical CVD or 10 year ASCVD risk<10% (BP goal<130/80) [25].
ESC 2018 Guidelines for Hypertension: It includes 10 point
strategy to:
Define: (>140/90 mmHg office BP)
and
Screen BP: (office and home readings)
Considering drug treatment of
hypertension:
Adults with Grade 1 hypertension (office BP 140-159/90-99) aged up 80 years,
should receive drug treatment if their BP is not controlled after a period of
lifestyle intervention alone. For high-risk patients with Grade 1 hypertension,
or patients with higher grades of hypertension (e.g., Grade 2 hypertension; ≥ 160/100 mmHg),
drug treatment should be initiated alongside lifestyle interventions.
Special considerations in
older patients:
For people over the age of 80 years, who have not yet received treatment for
their BP, BP treatment should be considered when office systolic BP is ≥ 160 mmHg.
How low should BP is lowered? A target range for treated
BP has been introduced. Office systolic BP should be lowered to<140 mmHg in
all treated patients, including independent older patients who can tolerate
treatment. The aim should be to target systolic BP to 130 mmHg for most
patients if tolerated.
Treatment of
hypertension-lifestyle interventions is important: The treatment of
hypertension involves lifestyle interventions and drug therapy. Lifestyle
interventions such as sodium restriction, alcohol moderation, healthy eating,
regular exercise, weight control, and smoking cessation are important.
Start treatment in most
patients with two drugs, not one: Monotherapy is usually inadequate therapy for most
people with hypertension Initial therapy with a combination of two drugs should
now be considered usual care for hypertension.
A single pill strategy to
treat hypertension: For better compliance single pill combination therapy is now the
preferred strategy for initial two-drug combination.
A simplified drug treatment
algorithm: A
combination of an ACE inhibitor or ARB with a CCB or thiazide/thiazide-like
diuretic is the preferred initial therapy for most patients. For those
requiring three drugs, a combination of an ACE-inhibitor or ARB with a CCB and
a thiazide/thiazide-like diuretic should be used. Beta blockers should be used
when there is a specific indication for their use, e.g. angina, post myocardial infarction, heart failure with reduced
ejection fraction, or when heart rate control is required.
Managing cardiovascular
disease risk in hypertensive patients-going beyond BP: Hypertensive patients
frequently have concomitant cardiovascular risk factors. Statin therapy should
be more commonly used in hypertensive patients with established cardiovascular
disease Benefit from statin therapy has also been observed in hypertensive
patients at the border between low and moderate risk. Antiplatelet therapy, especially low dose aspirin
is also indicated for secondary prevention in hypertensive patients but is not
recommended for primary prevention, i.e. in patients without cardiovascular
disease [26].
Mechanism of action of
various drugs: These
drugs reduce cardiac contractility, inhibit ACE activity, or promote diuresis.
None of these drugs focuses upon restoring cortical-hypothalamic signals or
bringing back VMC to a previous normotensive level. Centrally acting drugs are
not the first line in any guidelines. Centrally acting antihypertensive drugs
such as clonidine induce peripheral sympathoinhibition and a fall in blood
pressure as a result of alpha-2 adrenergic receptor agonist action in the brain
stem. Newer centrally acting drug Moxonidine in addition to alpha2 agonist has
an affinity for imidazoline receptor subtype 1, which reduces sympathetic
activity and blood pressure. It is suggested to be effective in cases where
other agents such as thiazides, beta-blockers, ACE inhibitors, and calcium channel blockers are not appropriate or
irresponsive [27].
Long term side effects of
antihypertensive therapy: Beta-blockers can cause bronchoconstriction, reduced cardiac output,
fatigue, heart block, dizziness, depression, bradycardia (decreased heartbeat and function), cold
extremities, poor circulation in the hands and feet), claudication, etc. CCBs
are associated with pedal edema, postural hypotension, headache, etc. Common side
effects of ACE inhibitors/ARBs are cough and angioneurotic edema and diuretics
are electrolyte imbalance and arrhythmia [28].
Results of Antihypertensive Treatment from a Few Previous Studies
Trends in Prevalence and
Control of Hypertension, 2017 American College of Cardiology/American Heart Association
(ACC/AHA) Guideline: The age-standardized proportion of controlled hypertension among adults
receiving antihypertensive pharmacologic treatment increased from 1999-2000
(25.6%) to 2015-2016 (43.5%). There was no consistent improvement in control
throughout the full period among non-Hispanic blacks, individuals aged>60,
or those with diabetes mellitus, chronic kidney disease or
high cardiovascular disease risk [7].
The global burden of
hypertension
analysis suggested that the number of adults with hypertension in 2025 was
predicted to increase by 60%. Hypertension is an important public health
challenge worldwide. Prevention detection, treatment, and control of this
condition should receive high priority [29].
Low dose triple pill (TRIUMPH Trial) lowers blood pressure more than usual care triple
therapy reduces blood pressure by 8.7 mmHg systolic v/s 4.5 for usual care [30].
In the United States, about 77.9 million (1 out of
every 3) adults have high blood pressure, Data from NHANES 2007-2010 showed
that of those with high blood pressure. 81.5 percent are aware they have high
BP. 74.9 percent are under current treatment. 52.5 percent are under control
and 47.5 percent are not under control [31,32].
Principal Results of the
(JATOS trial)
Japanese Trial to Assess Optimal Systolic Blood Pressure in Elderly Hypertensive
Patients-In this trial, the primary end point was the combined incidence of
cardiovascular disease and renal failure, and the secondary endpoints were
total deaths and any safety problems. Although final blood pressures
(systolic/diastolic) were significantly lower in the strict-treatment group
compared with the mild-treatment group (135.9/74.8 vs. 145.6/78.1 mmHg;
p<0.001), the incidence of the primary endpoint was similar in the two
groups (86 patients in each group; p=0.99). Total deaths were 54 in the
strict-treatment group vs. 42 in the mild-treatment group (p=0.22), and
treatment was withdrawn because of adverse events in 36 patients in each group
(p=0.99). An interaction between age and treatment for the primary endpoints
(p=0.03) was seen. Further studies are needed to assess the optimal treatment
strategy for hypertension in the elderly. There was also no significant group
difference in the secondary endpoints [33].
In clinical trials of
patients
with untreated hypertension and an average blood pressure of 155/100 mmHg,
treatment with 5 mg/80 mg per day of Nebivolol/valsartan for four weeks
resulted in an average reduction in systolic and diastolic blood pressures of 8.3 mmHg and 7.2 mmHg,
respectively. Higher doses did not typically improve blood pressure control [34,35].
Conclusions of various studies:
· Inadequate blood pressure control (mild to moderate control with 3-4 drugs i.e. 8-10 mmHg in the long term in systolic blood pressure, especially in elderly
· No significant difference in endpoints
· Continuous rise in the incidence of hypertension along with other comorbidities like diabetes, Dyslipidaemia, IHD (Ischemic Heart Disease), etc.
· Trials recommend the need for further studies to assess the optimal treatment strategy for hypertension in the elderly.
Side effects of therapy: After observing these facts do we need some other measures in lifestyle management besides available measures? To achieve better smooth control over hypertension. Possibly at all stages of hypertension with or without drug treatment, it must be directed to stress-relieving methods that reduce cortical influences; this, in turn, will help VMC to back to normal again. VMC will automatically correct various BP control mechanisms and bring back BP to normal. Drugs are, the primary way to control blood pressure at individual levels, but to control a global epidemic of hypertension; the better way is to improve lifestyle measures by reducing stress and mental exhaustion at a community level. There should be a bigger role and further work upon centrally acting drugs.
How to Bring Back VMC-Reset Cortical-Hypothalamic Signals-Is it Possible?
No clear answer/prospective results are available. This possibly requires continuous reduction/removal in mental stress/exhaustion. All efforts (relaxation methods given below) must be employed to relieve stress and exhaustion in lifestyle for hypertension besides JNC suggestions.
For mental exhaustion (burn out) from early
childhood; the following must be done-An adequate balance between mental work
and mental rest, avoid excess use of the laptop, mobile, computers and
television. Take good sound sleep for around 7 hours daily to rejuvenate neurotransmitters and reduce exhaustion.
Practice mental relaxation/Vipassana which helps to replenish the
neurotransmitters (Vipassana-state of complete mental silence i.e., no active
writing, reading, no speaking), it must be quantitative more the mental
exhaustion much theduration of Vipassana. Spend some time in the garden to
have tranquillity of mind. Practice sports/yogic exercises daily.
How relaxation techniques
help-Relaxation
(No active concentration) techniques, such as Shavasana, Makrasana, Vipassana
(relaxation postures where body and mind are allowed to relax) and sound sleep
relaxes the prefrontal network/lobe helps in replenishment of neurotransmitters
and helps in the integration/control of the other parts of the brain. Fatigue
of the prefrontal lobe/network increases distractibility by irrelevant stimuli
there is a reduced attention span and increased sympathetic activity.
For chronic stress and fast
mental speed
following must be done Try to avoid hurriedness in completing work, avoid
competitiveness, jealousy and high expectations in life. Practice meditation,
spend some time in nature; it reduces stress and fast mental speed. Practice
yogic exercises daily (Shavasana, Makrasana, few breathing exercises). Try to
divert the mind from stress thoughts by listening to soft music, light sports,
etc. Meditation is effective in reducing stress and fast mental speed.
How meditation acts-During meditation, the
person is asked to keep his concentration/attention at particular point (mostly
breath). The more the person can concentrate the less will he be disturbed by
external/ internal stimuli? Attention/concentration is an important function of
the prefrontal network (lobe) which acts as an integrator for other networks
(lobes) and helps in keeping attention. Meditation possibly improves overall
control of the prefrontal network (lobe) over other parts of the brain
including the hypothalamus thereby reducing sympathetic discharge to various
stimuli. All such above measures rejuvenate the brain and help in the
replenishment of neurotransmitters, synchronize cortical-hypothalamic signals, decrease basal sympathetic
discharge and help in the control of blood pressure (Flow chart 3) [10, 36-38].
Conclusions and Suggestions
High blood pressure is a state of vascular system where whole body vasculature is set at a higher level due to a higher setting of vasomotor center. This occurs due to desynchronized cortical-hypothalamic signals to the vasomotor center (stress, fast mental speed, and mental exhaustion). The outcome is increased basal sympathetic tone and hypertension. There is no substitute for a healthy lifestyle in preventing blood pressure mainly mental health (try to prevent to rise in sympathetic tone). This can be achieved by the prevention of stress, mental exhaustion and fast mental speed in daily life. Stress relaxation methods/adequate mental rest at regular intervals may also help. Dietary/drug therapy aimed at the use of nutritional supplements providing choline (helps in synthesis of acetylcholine in brain prevents mental exhaustion) and various alternate substances (supposed to reduce stress) like Brahmi (Bacopa monnieri) Shankhpushpi (Convolvulus pluricaulis) can also be used. More work is required for centrally acting drugs to be included as a regular part of therapy for hypertension [36].

Flow chart 3: Stress relaxation-VMC back to normal-Normal blood Pressure.
References
1. Egan B, Kjeldsen S, Grasi G, Esler M and Mancia G. The global burden of hypertension exceeds 1.4 billion people: should a systolic blood pressure target below 130 become the universal standard? (2019) J Hypertension 37: 1148-1153. https://doi.org/10.1097/hjh.0000000000002021
2. Singh AK and Mittal BV. Hypertension in the Developing World: Challenges and Opportunities (2010) Am J Kidney Dis 55: 590-598. https://doi.org/10.1053/i.ajkd.2009.06.044
3. Reid CM and Thrift AG. Hypertension 2020: confronting tomorrows problem today (2005) Clin Exp Pharmacol Physiol 32: 374-376. https://doi.org/10.1111/j.1440-1681.2005.04199.x
4. Saxena T, Ali AO and Saxena M. Pathophysiology of essential hypertension: an update (2018) Expert Rev Cardiovasc Ther 16: 879-887. https://doi.org/10.1080/14779072.2018.1540301
5. Chobanian AV, Bakris GL, Black HR, Cushman WC, Green LA, et al. Seventh report of the joint national committee on prevention, detection, evaluation, and treatment of high blood pressure, the JNC 7 report (2003) JAMA 21: 2560-2572. https://doi.org/10.1001/jama.289.19.2560
6. James PA, Oparil S, Carter BL, Cushman WC, Dennison-Himmelfarb C, et al. 2014 evidence-based guideline for the management of high blood pressure in adults: report from the panel members appointed to the Eighth Joint National Committee (JNC 8) (2014) JAMA 311: 507-520. https://doi.org/10.1001/jama.2013.284427
7. Dorans SK, Mills TK, Liu Y and Jiang He. Trends in Prevalence and Control of Hypertension according to the 2017 American College of Cardiology/American Heart Association (ACC/AHA) Guideline (2018) J Am Heart Association 7: e008888. https://doi.org/10.1161/jaha.118.008888
8. Guyton AC and Hall JE. The autonomic nervous system. In: Textbook of medical physiology (13th Edn) (2016) Philadelphia: Elsevier 832-834.
9. Saxena T and Saxena M. Possible clinical implications of high left ventricular ejection force and exaggerated sympathetic skin response (2016) Ann Clin Exp Hypertension 4: 1035.
10. Saxena T and Mittal SR. Stress relaxation in management of mild to moderate hypertension (2000) Asian J Clin Cardiol 2: 36-41.
11. Hart EC and Charkoudian N. Sympathetic neural mechanisms in human blood pressure regulation (2011) Curr Hypertens Rep 13: 237-243. https://doi.org/10.1007/s11906-011-0191-1
12. Padmanabhan TNC, Dani S, Chopra VK, Guha S, Vasnawala H, et al. Prevalence of sympathetic over activity in hypertensive patients-A pan India, non-interventional, cross-sectional study (2014) Ind Heart J 66: 686. https://doi.org/10.1016/j.ihj.2014.10.421
13. Padmanabhan S, Aman A and Dominiczak AF. Genomics of hypertension (2017) Pharmacol Res 121: 219-229. https://doi.org/10.1016/j.phrs.2017.04.031
14. Fuentes RM, Notkola IL, Semeikka S, Tuomilehto J and Nissinen A. Familial aggregation of blood pressure: a population-based family study in eastern Finland (2000) J Hum Hypertension 14: 441-445. https://doi.org/10.1038/sj.jhh.1001049
15. Katori M and Majima M. A missing link between high salt intake and blood pressure increase (2006) J Pharmacol Sci 100: 370-390. https://doi.org/10.1254/jphs.crj06003x
16. De Leeuw PW and Kroon AA. Abnormal pressure-natriuresis in hypertension: role of nitric oxide (2013) Acta Physiol Scand 62: 461-462.
17. Wofford MR and Hall JE. Pathophysiology and treatment of obesity hypertension (2004) Curr Pharm Des 10: 3621-3716. https://doi.org/10.2174/1381612043382855
18. Leuenberger U, Jacob E, Sweer L, Waravdekar N, Zwillich C, et al. Surges of muscle sympathetic nerve activity during obstructive apnea are linked to hypoxemia (1995) J Appl Physiol 79: 581-587. https://doi.org/10.1152/jappl.1995.79.2.581
19. Schulman IH and Zhou MS. Vascular insulin resistance: a potential link between cardiovascular and metabolic diseases (2009) Curr Hypertens Rep 11: 48-57. https://doi.org/10.1007/s11906-009-0010-0
20. Luscher TF, Noll G and Nava E. Endothelial Dysfunction and Hypertension (2014) Vascular Endothelium Human Physiol Pathophysiol 125-146.
21. Saxena T, Patidar S, Verma S, Ali OA and Saxena M. Endothelial Cells Strengthening: Improving Functions in Management of Acute Coronary Syndrome (A Double-Blind Randomized Interventional Control Trial) (2019) Clinical Cardiol Cardiovascular Med 3: 14-19. https://doi.org/10.33805/2639.6807.120
22. Cooper SA, Whaley-Connell A, Habibi J, Wei Y, Lastra G, et al. Renin-angiotensin-aldosterone system and oxidative stress in cardiovascular insulin resistance (2007) Am J Physiol Heart Circ Physiol 293: H2009-H2023. https://doi.org/10.1152/ajpheart.00522.2007
23. Engeli S, Negrel R and Sharma AM. Physiology and pathophysiology of the adipose tissue renin-angiotensin system (2000) Hypertension 35: 1270-1277. https://doi.org/10.1161/01.hyp.35.6.1270
24. Saxena T, Patidar S and Saxena M. Assessment of left ventricular ejection force and sympathetic skin response in normotensive and hypertensive subjects: A double-blind observational comparative case-control study (2016) Ind Heart J 68: 685-692. https://doi.org/10.1016/j.ihj.2015.12.005
25. Whelton KP, Carey MR, Aronow SW, Casey ED, Collins JK, et al. 2017 ACC/AHA/AAPA/ABC/ACPM/AGS/APhA/ASH/ASPC/NMA/PCNA Guideline for the Prevention, Detection, Evaluation, and Management of High Blood Pressure in Adults: Executive Summary: A Report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines (2018) Hypertension 71: 1269-1324. https://doi.org/10.1161/HYP.0000000000000066
26. Williams B. Ten Commandants of the 2018 ESC/ESH HTN Guidelines on Hypertension in Adults (2018) Europen Heart J 39: 3007-3008. https://doi.org/10.1093/eurheartj/ehy439
27. Fenton C, Keating GM and Lyseng-Williamson KA. Moxonidine: a review of its use in essential hypertension (2006) Drugs. https://doi.org/10.2165/00003495-200666040-00006
28. Loga-Zec S, Asceric M, Loga-Andrijic N, Kapetanovic B and Zerem E. The Incidences of antihypertensive Drug-induced Side Effects in Patients with Diabetes Mellitus Type 2 and Hypertension (2014) 68: 372-375. https://doi.org/10.5455/medarh.2014.68.372-375
29. Kearney PM, Whelton M, Reynolds K, Muntner P, Whelton PK, et al. Global burden of hypertension: analysis of worldwide data (2017) Lancet 389: 37-55. https://doi.org/10.1016/S0140-6736(05)17741-1
30. TRIUMPH: Low-Dose Combination Pill Lowers Blood Pressure more than usual care.
31. Prevalence of High Blood Pressure in adults Age 20 and Older NHANES 2007-2010.
32. Keenan NL, Rosendorf KA and Centers for Disease Control and Prevention (CDC). Prevalence of hypertension and controlled hypertension-United States, 2005-2008 (2011) MMWR Suppl 60: 94-97.
33. JATOS Study Group. Principal results of the Japanese trial to assess optimal systolic blood pressure in elderly hypertensive patients (JATOS) (2008) Hypertens Res 31: 2115-2127. https://doi.org/10.1291/hypres.31.2115
34. Sander GE, Fernandez C and Giles TD. Fixed-dose combination therapy of nebivolol and valsartan for the treatment of hypertension (2016) Expert Rev Cardiovasc Ther 14: 563-572. https://doi.org/10.1586/14779072.2016.1167598
35. Ishak J, Rael M, Punzi H, Gradman A, Anderson MY, et al. Additivity of nebivolol/valsartan single-pill combination versus other singles- pill combinations for hypertension (2018) J Clin Hypertens 20: 143-149. https://doi.org/10.1111/jch.13132
36. Saxena T, Maheshwari S and Saxena M. Aetiopathogenesis of type-2 diabetes mellitus; could chronic stress play an important role (2014) J Assoc Physicians India 62: 484-489.
37. Saxena T, Patidar S, Ali OA, Saxena M and Kabra M. Effect of various Stress Relaxation Exercises on Electroencephalography, Sympathetic Skin Response and Type-2 Diabetes Mellitus (2018) Arch Endocrinol Diabetes Care 2: 164-175.
38. Saxena T, Ali OA and Saxena M. Lifestyle Management in Diabetes (2019) Diabetes Complications 3: 1-2.
Corresponding author:
Tarun Saxena, Senior Consultant, Department of Internal Medicine, Mittal Hospital and Research Centre, Ajmer, Rajasthan, India, Tel: +91-9829089284, E-mail: yogdiab@gmail.com
Citation:
Saxena T, Saxena A, Ali OA and Saxena M. Vasomotor center? a possible role in the treatment of hypertension (2019) Clinical Cardiol Cardiovascular Med 3: 37-42.
Keywords
Vasomotor Center, Hypertension, Cardiac failure, Renal failure and Cardiovascular disease.


 PDF
PDF