Introduction
The initial
presentation of a novel Coronavirus-2 (COVID-19) that is resulting in Severe
Acute Respiratory Syndrome (SARS) had appeared in Wuhan, China in December 2019
[1]. COVID-19 Disease is a highly communicable, rapidly spread, lethal
worldwide disease [2]. Despite COVID-19 disease was primarily presented with
respiratory symptoms, but cardiovascular involvements were common and
accompanied by higher mortality among these patients [3]. However, cardiac
manifestations represent a late phenomenon of the viral respiratory infection
in COVID-19 patients. Myocardial infarction, arrhythmias, cardiac arrests,
Heart Failure (HF), and Venous Thromboembolism (VTE) are frequent
cardiovascular complications in COVID-19 patients that is varying from 7.2% up
to 33% [3]. Arrhythmias are commonly recognized sequel in COVID-19 patients,
with Atrial Fibrillation (AF) being the most common form. An electrical,
calcium handling and structural remodeling have represented keystone in
understanding AF pathogenesis [4].
The clinical
manifestations of AF are highly variable and the actual mechanisms of AF are
still vague in a big sector of patients [5]. The underlying pathogenesis of AF
in COVID-19 patients is still idiopathic [4]. According to current literature,
AF was detected in 19% to 21% among COVID-19 patients [4]. The incidence of AF
is usually high in patients with severe pneumonia, SARS, septic shock, and the
during hospitalization [4]. According to the Danish Nationwide Registry (DNR),
new-onset AF was reduced by 47% in the first three weeks of the national
lockdown in comparison with the simultaneously the past year [6]. A reduction
in angiotensin-converting enzyme 2 (ACE-2) receptor availability, CD147 and
sialic acid-spike protein reaction, increased inflammatory signaling
subsequently culmination in an inflammatory cytokine storm, direct viral
endothelial damage, acute electrolytes disturbance, acute acid-base imbalance,
and increased adrenergic drive are proposed putative mechanisms in the
pathophysiology of COVID-19 related-AF [7].
Currently, therapy of
AF with Antiarrhythmic Drugs (AADs), and anticoagulants are complex,
suboptimal, and are accompanied by anxious side effects [4]. Acute Coronary
Syndrome (ACS) due to a Coronary Artery Spasm (CAS) can occur in a severe acute
respiratory syndrome in COVID-19 patients [8]. Despite the actual mechanisms of
CAS in COVID-19 patients are multifaceted, but, it still unknown.
Hypercontractillity of coronary smooth muscle is usually induced by a rise of
IC calcium (CA++) especially with elevated CA++ sensitivity are proposed
mechanisms in understanding COVID-19 virus-inducing CAS [8]. However, CAS may
occur in patients with established atherosclerotic coronary lesions.
Importantly, inflammatory processes, IL-6 polymorphism, and oxidative stress
may implicate in the pathogenesis of COVID-19 virus-inducing CAS [9]. Moreover,
a major systemic inflammatory response, endothelial dysfunction, and activation
of the ACE-2 receptor may play a role in inducing coronary artery spasm in COVID-19
infection [10].
Wavy triple an electrocardiographic sign (Yasser Sign) is a new innovated diagnostic sign in hypocalcaemia [11]. The author interpretations for this sign are based on the following;
- Different successive three beats in the same lead are affected.
- A Wavy triple sign can affect all ECG leads.
- An associated elevated beat is seen with the first of the successive three beats, a depressing beat with the second beat, and an isoelectric ST-segment in the third one.
- The elevated beat is either accompanied by ST-segment elevation or just an elevated beat above the isoelectric line.
- Also, the depressed beat is either associated with ST-segment a depressing or just depressed beat below the isoelectric line.
- The configuration for depressions, elevations, and isoelectric ST-segment for the subsequent three beats is variable from case to case.
So, this arrangement is
non-conditional. This is meaning the sign conditionally no affect specific ECG
partition e.g., inferior, anterior, or lateral, etc. Mostly, there is no
participation among the involved leads. Thus, the sign is not conditionally
included in an especial coronary artery for the affected leads [11].
Case Presentation
A 60-year-old married
male, farmer, Egyptian patient presented to the Physician Outpatient Clinic (POC)
with acute tachypnea, chest pain, and palpitations. Fatigue, loss of appetite,
and generalized body aches were associated symptoms. He gave a history of
tachypnea for 4 days. Informed consent has been signed by the patient but
unfortunately, there was no ethical approval. Currently, he had a history of
contact in the past 7 days with his son who confirmed a COVID-19 patient. Upon
general physical examination; generally, the patient was tachypneic,
distressed, with an irregular pulse rate (atrial fibrillation of VR of 160),
blood pressure (BP) of 140/80 mmHg, respiratory rate of 40 bpm, the temperature
of 39.5°C, and pulse oximeter of oxygen (O2) saturation
of 88%. He seemed thin and long. No more relevant clinical data were noted
during the physical examination.
The patient was treated at home with COVID-19 pneumonia, atrial fibrillation, coronary spasm, and Wavy triple sign or Yasser’s sign. Initially, the patient was treated with O2 inhalation by O2 cylinder (100%, by nasal cannula, 5L/min). The patient was maintain treated with cefotaxime; (1000 mg IV every 8hours), azithromycin (500 mg PO single daily dose), oseltamivir (75 mg PO twice daily only for 5 days), and paracetamol (500 mg IV every 8 hours as needed). SC enoxaparin 80 mg twice daily), aspirin tablet (75 mg, once daily), clopidogrel tablet (75 mg, once daily), diltiazem tablet (60 mg, once daily), and hydrocortisone sodium succinate (100 mg IV every 12 hours) were added. The patient was daily monitored for temperature, pulse, blood pressure, and O2 saturation. The initial ECG on presentation showing atrial fibrillation (of VR of 160) with a T-wave inversion in inferior leads (II, III, and aVF), in anterior leads (V4-6 leads), and an upright T-wave in aVR lead. There is a Wavy triple sign of hypocalcaemia or Yasser’s sign-in V1-3 leads (Figure 1A).
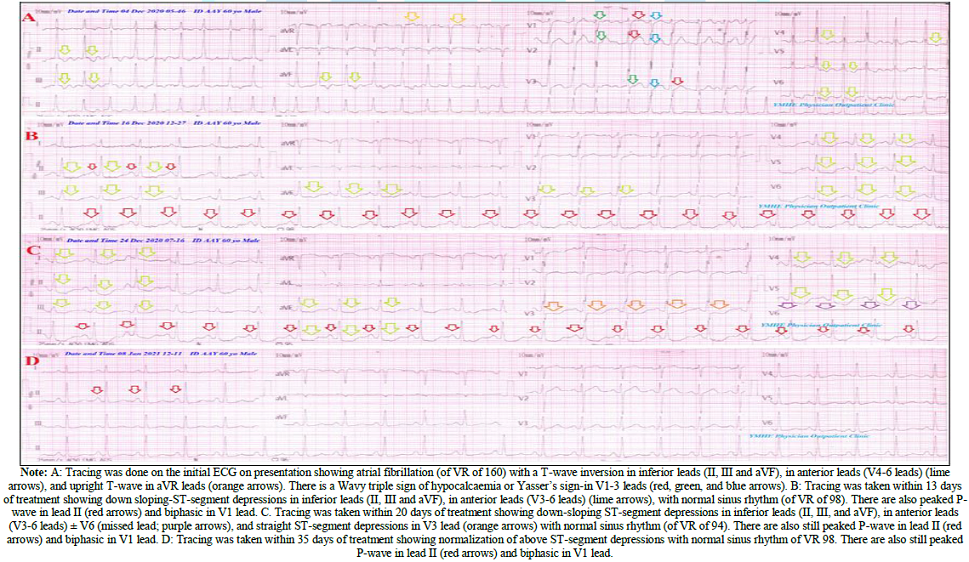
Figure 1: Serial ECG tracings.
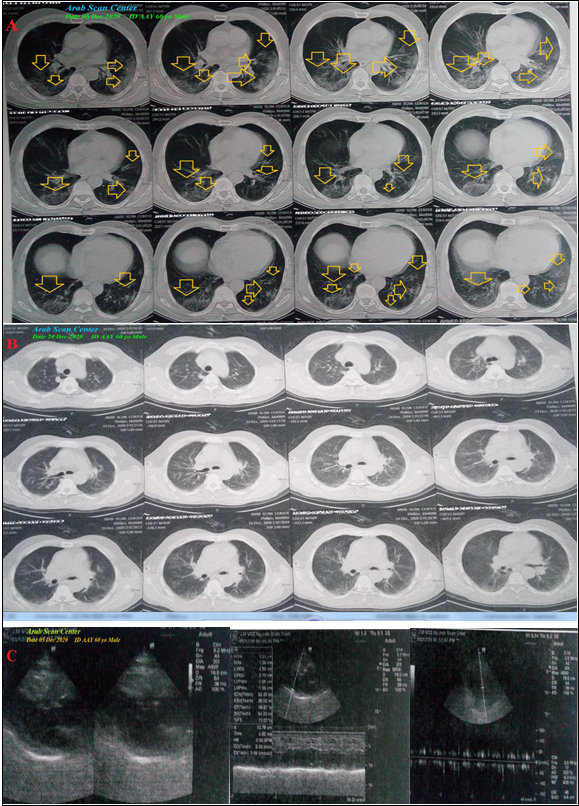
Figure 2: A: Chest CT scan was done on presentation showing bilateral multiple
The patient was tested
for latent tetany which was positive. The initial Complete Blood Count (CBC);
Hb was 14.2 g/dl, RBCs; 4.83*103/mm3, WBCs; 5.29*103/mm3
(Neutrophils; 76%, Lymphocytes: 20%, Monocytes; 3%, Eosinophils; 1% and
Basophils 0%), Platelets; 142*103/mm3. S. Ferritin was high; 547
ng/ml. D-dimer was high (563 ng/ml). CRP was high; 48 g/dl. LDH was high; 776
U/L. SGPT was normal; 25 U/L, SGOT was normal; 42 U/L. Serum creatinine showed
mild elevation; 1.5 mg/dl and blood urea; showed mild elevation; 110.7 mg/dl
was high. RBS was; 91 mg/dl. Ionized calcium was mildly low; 0.71 mmol/L.
The troponin test was
positive. After 21 days of management; RBS was normal; 119 mg/dl. CBC; Hb was
12.7 g/dl, RBCs; 4.29*103/mm3, WBCs; 5.84*103/mm3
(Neutrophils: 68%, Lymphocytes: 25%, Monocytes: 6%, Eosinophils: 1% and
Basophils: 0%), Platelets: 85*103/mm3. Serum ferritin was normal;
291 ng/ml. D-dimer was normal (100 ng/ml), CRP was negative (0.4 g/dl), LDH was
still high; 624.94 U/L. SGPT was normal; 19 U/L, SGOT was normal; 37 U/L. Serum
creatinine; 1.3 mg/dl and blood urea; 49.4 mg/dl were normal. Ionized calcium
was normal; 1.23 mmol/L. The troponin test had become negative. The first chest
CT scan was done on presentation showing bilateral multiple patchy ground-glass
pulmonary consolidations (Figure 2A).
Serial ECG tracings were done. ECG tracing was taken within 13 days of
treatment showing down-sloping ST-segment depressions in inferior leads (II,
III, and aVF), in anterior leads (V3-6 leads), with normal sinus rhythm (of VR
of 98).
There are also peaked
P-wave in lead II and biphasic in V1 lead (Figure
1B). ECG tracing was taken within 20 days of treatment showing down-sloping
ST-segment depressions in inferior leads (II, III, and aVF), in anterior leads
(V3-6 leads) ± V6 (missed lead), and straight ST-segment depressions in V3 lead
with normal sinus rhythm (of VR of 94). There are also still peaked P-wave in
lead II and biphasic in V1 lead (Figure
1C). An oral nitroglycerine capsule (2.5 mg, twice daily) was added. The
last chest CT scan was done within 20 days of the presentation showing nearly
dramatic improvement of the above ground-glass consolidations (Figure 2B). Echocardiography showed no
detected abnormality with an EF of 58% (Figure
2C). COVID-19 pneumonia with coronary artery spasm and the Wavy triple an
electrocardiographic sign (Yasser Sign) was the most probable diagnosis.
ECG tracing was taken
within 35 days of treatment showing normalization of above ST-segment
depressions with normal sinus rhythm of VR 98. There are also still peaked
P-wave in lead II and biphasic in V1 lead. (Figure 1D). Within 24 days of the above management, the patient
finally showed nearly complete clinical, radiological, and laboratory
improvement. The patient was continued on aspirin tablet (75 mg, once daily),
oral nitroglycerine capsule (2.5 mg, twice daily) and diltiazem tablet (60 mg,
once daily), oral calcium, and vitamin-D preparation for 30 days with further
recommended cardiac and chest follow up.
Discussion
Overview:
An elderly farmer male COVID-19 patient presented to physician outpatient
clinic with bilateral pneumonia, AF, evidence of coronary artery spasm, and
Wavy triple an electrocardiographic (ECG) sign or Yasser Sign of hypocalcemia.
The objective primary for my case study was the presence of COVID-19 pneumonia, AF, evidence of coronary artery spasm, and Wavy triple an ECG sign (Yasser Sign) of hypocalcemia in POC.
The secondary objective
for my case study was the question of; How did you manage the case?
- There was a history of direct contact to confirmed the COVID-19 case.
- The presence of direct contact to confirmed the COVID-19 case, and bilateral ground-glass consolidation on top of acute tachypnea will strengthen the COVID-19 diagnosis.
- The tachypnea, hypoxia, consolidation, electrocardiographic P-pulmonal, and elevated d-dimer are highly suggestive of associated pulmonary embolism.
- An associated marked elevated d-dimer, IHD, and hypocalcemia in the COVID-19 case presentation may carry a bad prognostic outcome and is indicating a high-risk condition.
- There is a dramatic reversal of ST-segment depressions in a COVID-19 patient after adding oral nitroglycerine is an indicator for the presence of coronary artery spasm.
- The presence of ST-segment depressions in ECG may be interpreted as accompanied by severe specific ischemic myocardial insult.
- The dramatic reversal of ST-segment depressions in ECG may be interpreted as a coronary artery spasm. Hypoxia and suspected pulmonary embolism were possible mechanisms.
- The disappearance of AF after initial therapy may a guide for a good prognosis in this case study.
- The spontaneous evanescence of Wavy triple electrocardiographic sign from ECG V1-3 leads is a hallmark for the existence of the Movable-weaning phenomenon of hypocalcemia. Tachypnea was a possible cause of hypocalcemia and subsequent Wavy triple electrocardiographic and Movable-weaning phenomenon of hypocalcemia [11,12].
- A nearly complete clinical, radiological, and laboratory improvement that occurred after the management with anti-infective drugs, anticoagulants, steroids, and antiplatelet strongly implies their effects.
- The normal lymphocytic count does not exclude COVID-19 infection. But it carries a good prognosis.
- Blood pressure, respiratory rate, pulse, and O2 saturation are a strong guide for clinical follow-up in COVID-19 patients.
- A gradual decreasing the level of elevated CRP, d-dimer, and serum ferritin may be used as another good laboratory guide for follow-up for COVID-19 pneumonic patients.
- The serial change of radiological changes from normal chest CT to abnormal to normal at the end will strengthen the effectiveness of used drugs in this management.
I can’t compare the
current case with similar conditions. There are no similar or known cases with
the same management for near comparison.
The only limitation of
the current study was the unavailability of the invasive test for coronary
artery spasm.
Conclusion and Recommendations
- It signifies the role of the anti-infective drugs, anticoagulants, antiplatelet, and steroids in COVID-19 patients with bilateral pneumonia, AF, coronary artery spasm are effective therapies.
- The disappearance of AF after initial therapy may a guide for a good prognosis in this case study.
- The evanescence of Wavy triple ECG sign as a hallmark for the existence of the Movable-weaning phenomenon of hypocalcaemia is recommended for further wide-study.
References
- Zhu N, Zhang D, Wang W, Li X, Yang B, et al. A novel coronavirus from patients with pneumonia in China, 2019 (2020) N Engl J Med. 382:727-733.
- WHO. Coronavirus disease 2019 (COVID-19) Situation Report-165 (2020).
- Kwenandar F, Japar KV, Damay V, Hariyanto TI, Tanaka M, et al. Coronavirus disease 2019 and cardiovascular system: A narrative review (2020). Int J Cardiol Heart Vasc 29. https://doi.org/10.1016/j.ijcha.2020.100557
- Gawalko M, Kaplon CA, Hohl M, Dobrev D, Linz D. COVID-19 associated atrial fibrillation: Incidence, putative mechanisms and potential clinical implications (2020) Int J Cardiol Heart Vasc 30. https://doi.org/10.1016/j.ijcha.2020.100631
- Andrade J, Khairy P, Dobrev D, Nattel S. The clinical profile and pathophysiology of atrial fibrillation: relationships among clinical features, epidemiology, and mechanisms (2014) Circ Res 114:1453-1468. https://doi.org/10.1161/circresaha.114.303211
- Holt A, Gislason GH, Schou M, Zareini B, Biering ST, et al. New-onset atrial fibrillation: incidence, characteristics, and related events following a national COVID-19 lockdown of 5.6 million people (2020) Eur Heart J 41:3072-3079. https://doi.org/10.1093/eurheartj/ehaa494
- Kochi AN, Tagliari AP, Forleo GB, Fassini GM, Tondo C. Cardiac and arrhythmic complications in patients with COVID-19 (2020) J Cardiovasc Electrophysiol 31: 1003-1008. https://doi.org/10.1111/jce.14479
- Rivero F, Antuña P, Cuesta J, Alfonso F. Severe coronary spasm in a COVID-19 patient (2020) Catheter Cardiovasc Interv 97: 670-672. https://doi.org/10.1002/ccd.29056
- Murase Y, Yamada Y, Hirashiki A, Ichihara S, Kanda H, et al. Genetic risk and gene-environment interaction in coronary artery spasm in Japanese men and women (2004) Eur Heart J 25: 970-977. https://doi.org/10.1016/j.ehj.2004.02.020
- Tavazzi G, Pellegrini C, Maurelli M, Belliato M, Sciutti F, et al. Myocardial localization of coronavirus in COVID-19 cardiogenic shock (2020) Eur J Heart Fail 22: 911-915. https://doi.org/10.1002/ejhf.1828
- Elsayed YMH. Wavy Triple an Electrocardiographic Sign (Yasser Sign) in Hypocalcemia. A Novel Diagnostic Sign; Retrospective Observational Study (2019) EC Emergency Medicine and Critical Care 3:1-20.
- Elsayed YMH. Movable-Weaning off an Electrocardiographic Phenomenon in Hypocalcemia (Changeable Phenomenon or Yasser’s Phenomenon of Hypocalcemia)-Retrospective-Observational Study (2020) CPQ Medicine 11.
*Corresponding author:
Yasser
Mohammed Hassanain Elsayed, Critical Care Unit, Fraskour Central Hospital,
Damietta Health Affairs, Egyptian Ministry of Health (MOH), Damietta, Egypt,
Email: dryaser24@yahoo.com
Citation:
Elsayed Y.M.H. COVID-19 pneumonia with atrial fibrillation, coronary spasm, and wavy triple sign (Yasser’s sign); dramatic reversal at home management (2021) Clinical Cardiol Cardiovascular Med 4: 20-23.
Keywords
COVID-19, Coronavirus, Bilateral pneumonia,
Atrial fibrillation, Wavy triple electrocardiographic sign, Movable-weaning
phenomenon.


 PDF
PDF